Efficacy of the new haemodialysis techniques:
In vitro comparison of pre- and post-dilutional haemodiafiltration
Alain Ficheux and Àngel Argilés *
UDSA-AIDER and
Institut de Génétique Humaine – UPR 1124 C.N.R.S.
746, Rue croix de Lavit
34192 Montpellier Cedex 5. France
* To whom correspondence and reprint requests may be sent angel.argiles@igh.cnrs.fr
Introduction
New renal replacement techniques aim to improve the clearances of small as well as large molecules. It is accepted that diffusive methods mostly influence low molecular weight solutes whereas high molecular weight components are preferentially driven by convective forces. Haemodiafiltration is one of the most efficient dialysis techniques presently available, which incorporates both diffusive and convective forces (1).
In post-dilutional haemodiafiltration the removed plasma is partially replaced after the haemodialyser, just before returning the blood to the patient. However, increasing ultrafiltration rate results in increased concentration of the retained elements - mainly the cellular component of blood - within the dialyser. This haemoconcentration with its associated increase in viscosity as blood passess through the dialyser may become a limiting factor of the amount of convectional mass transfer that may be achieved with post-dilutional techniques. Pre-dilutional haemodiafiltration and haemofiltration, which re-inject the replacement fluid before the dialyser obviate the haemoconcentration phenomenon and extend the range of blood flow and ultrafiltration rate that are allowed in vivo (2).
However, the precise benefits of the convective flow used in on-line haemodiafiltration, and particularly the differences in efficiency between pre and post-dilutional haemodiafiltration have not been well quantified.
The aim of this study was to evaluate the final clearances of small solutes in haemodiafiltration and compare pre- versus post-dilutional haemodiafiltration. To precisely evaluate total clearances in both haemodiafiltration settings we built an " in vitro " system, which enabled us to easily modify QB, QD, convection volume, as well as the infusion site (pre or post-dilutional). This system has been previously validated and described elsewhere (3).
Materials and Methods
Total ion clearance was used as a surrogate of urea clearance to evaluate the efficacy of dialysis techniques based on previous studies (4,5). In the present study we determined total ion clearance in the absence of net ultrafiltration according to the following formula:
Clearance = Dialysance = QD x ( CDi - CDo )/ CDi
C = concentration of total ion
QD = total dialysate flow produced by the system
(QD= QDi (at dialysate inlet) + Qinf (infusion flow))
Di = dialysate inlet
Do = dialysate outlet
The measured conductivity, was used to obtain the concentration value following our experimental data.
RC= 0.000381*S^2 + 0.066217*S - 0.020226
RC = Relative Concentration
S = Conductivity (mS/cm)
The in vitro system is described in Figure 1. A dialysis monitor with a volumetric ultrafiltration controller was used. Therefore, changing the flow setting of the infusion pump could easily and precisely modify the convection volume per time unit. Accordingly, convective flow was varied in this study by modifying infusion flow rate.
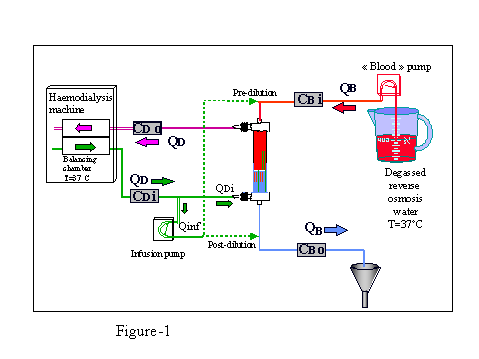 Degassed, reverse osmosis, warmed water was used for the blood compartment fluid. Precise QD and QB were checked by collecting the volumes over a time period before and at the end of each series of measurements. Three repeats were performed for each control point.
Degassed, reverse osmosis, warmed water was used for the blood compartment fluid. Precise QD and QB were checked by collecting the volumes over a time period before and at the end of each series of measurements. Three repeats were performed for each control point.
Study protocol
A cellulose triacetate dialyser of 1.70 m² was used in this study, (FB-170 U, Nipro, NISSHO Corporation, Osaka, Japan). Three different dialysers were used and three repeats were performed in each separate experiment for every data point of the study. The mean value of the separate experiments was used for analysis.
The influence of dialysate and blood flows was measured both as an internal control of the in vitro setting and to evaluate the magnitude of the influence of these parameters on the final clearance. The blood flows tested ranged from 250 to 450 ml/min in order to mimic the in vivo dialysis. The dialysate flows assessed ranged from 420 to 970 ml/min.
Infusion site. The main point of the study was the comparison between pre- and post-diafiltration. The precise infusion sites for both techniques are depicted in dotted lines in Fig 1.
Statistics. Values are given as the mean ±
standard error of the mean.
Results
QB influence on total ion clearance. Fig 2-a depicts the influence of the increase in QB from 250 to 450 ml/min, both with QD=620 ml/min and QD=970 ml/min on total ion clearance. An increase on QB resulted in an increase in total ion clearance from 228±
1 to 336±
1 ml/min with a QD = 620 ml/min. When QD was increased to 970 ml/min the final clearance was similar to that observed with QD = 620 ml/min for low QB levels (250 ml/min) and differed while increasing QB (Fig 2-a).
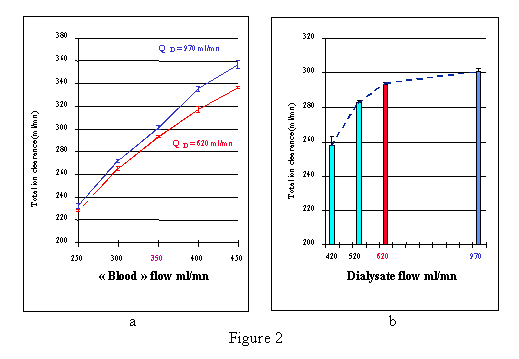 QD influence on total ion clearance. Figure 2-b depicts the experiments performed with a range of QD from 420 to 970 ml/min. For a fixed QB = 350 ml/min the total ion clearance increased from 258±5 to 301±1 ml/min (Fig 2-b).
QD influence on total ion clearance. Figure 2-b depicts the experiments performed with a range of QD from 420 to 970 ml/min. For a fixed QB = 350 ml/min the total ion clearance increased from 258±5 to 301±1 ml/min (Fig 2-b).
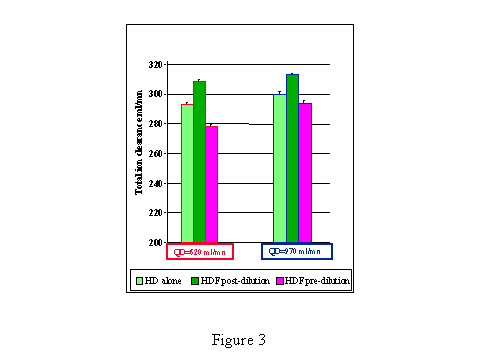
Infusion site study. Isolated dialysis as well as 100 ml/min of added convection in pre- and post-dilutional haemodiafiltration for a fixed QB=350 ml/min with total dialysate fluid (QD) production maintained at either 620 or 970 ml/min are presented in figure 3. Infusion of the replacement fluid in post-dilutional diafiltration resulted in a significant increase in total ion clearance. The opposite was observed when the replacement fluid was injected before the dialyser in pre-dilutional diafiltration.
Infusate volume study. We assessed a range of infusion rate from 0 (isolated dialysis) to 200 ml/min (reasonable maximum used in clinical practice). With post-dilutional haemodiafiltration we observed a linear increase in total ion clearance, whilst with pre-dilutional haemodiafiltration we obtained a linear decrease in total ion clearance (Figure 4-a).
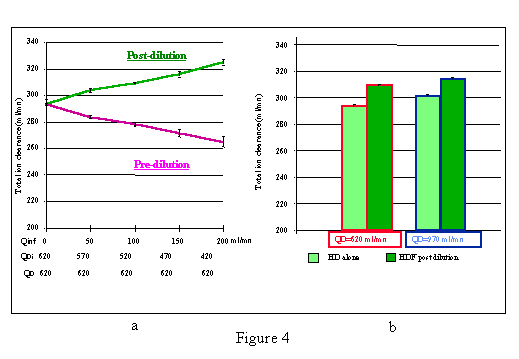
Comparison of dialysis efficacy using 620 and 970 ml/min of total dialysate production flow both with isolated dialysis and post-dilutional diafiltration. The results are depicted in fig 4-b. Again, total ion clearances were significantly increased with 100 ml/min post-dilutional infusion both at 620 and 970 ml/min of QD. When comparing the absolute values of the different experiments it can be observed that post-dilutional haemodiafiltration with a total QD production of 620 results in a higher total ion clearance than isolated dialysis with a total QD of 970 ml/min. The addition of post-dilutional infusion in the higher QD resulted in a further increase in total ion clearance, this being the most efficient setting of those we assessed.
Discussion
Following the policies of renal replacement therapy applied in most countries, it is becoming more and more important to evaluate the cost-effectiveness of different treatments. This fully applies for haemodiafiltration since it is an expensive technique that is supposed to improve dialysis efficacy. On-line haemodiafiltration was conceived to limit the spending increase associated to the use of manufactured infusion fluids for haemodiafiltration and to allow unlimited convection volumes (6). Besides to minimising the added costs inherent to haemodiafiltration, it is therefore important to properly evaluate the efficacy of this system.
The present study clearly shows that post-dilutional haemodiafiltration results in a significant increase in the clearance of small molecular weight components and that this increase is proportional to the amount of convection added. Interestingly, it also shows that pre-dilutional haemodiafiltration follows an opposite tendency. Increasing convection, with its associated increase in the infusion of the replacement fluid before the dialyser, decreases also proportionally, the efficacy in clearing small molecular weight solutes.
While the increased clearances associated to post-dilutional haemodiafiltration are well known and taken profit of in clinic, the information concerning the modifications in the efficacy of pre-dilutional haemodiafiltration is scant. Only two studies have previously reported that pre-dilutional haemodiafiltration may actually be less effective than simple haemodialysis. Ahrenholz et al (7) assessed the clearance of a variety of substances with different molecular weight in a limited number of convection settings in pre-dilutional haemodiafiltration and found that total clearance tended to decrease in pre-dilutional haemodiafiltration (7). In our studies (3 and the present data), we assessed an extended convection range and found that the decrease in total clearance seemed to have a linear distribution (3). Very recently, we have confirmed the linearity of this distribution and provided the simplified formula to calculate total clearance of small molecular weight solutes in haemodiafiltration (8). All these studies confirm that in on-line pre-dilutional haemodiafiltration, the more we increase convection, the less we will be clearing small molecular weight solutes (3,7,8).
In our institution we have been using on-line post-dilutional haemodiafiltration since 1990 with very high removal of both small as well as high mol wt compounds (9). With the flow rates employed (typically 100 ml/min) the average measured Kt/V urea is 1.7 ±
0.2 and as we have reported previously the reduction of serum b2-microglobulin is over 60% for a haemodiafiltration session (10). However, we are limited in the convective volume by the induced haemoconcentration, particularly in those patients with high haematocrite level. Thus, pre-dilutional haemodiafiltration was considered, but rejected on the grounds of the data presented in this study.
Taking together the results of the present experiments, the cost-effective comparison of the different haemodialysis settings shows that on-line post-dilutional diafiltration results in a superior performance. It is noteworthy, that the increase in dialyser clearance induced by 100ml/min of convection, for a total diaysate production of 620 ml/min is ~8 % (for 350 ml/min of QB). This value is significantly higher than that obtained with a 50% increase in dialysate flows and normal dialysis (970 ml/min of total dialysate produced and spent). Therefore, for a better efficiency, the savings of post-dilutional haemodiafiltration are evident.
Acknowledgements. We want to thank Drs Jean-Yves Bosc, Ronan Lorho, Carlos Vela, Jean-Louis Flavier, Bernard Canaud, Laurie J. Garred, Peter G. Kerr, Jean-Luc Fabre and Charles Mion for their constructive discussions on the studies included in this paper. The contents of this paper have been mostly taken and modified from our work published in Blood Purification 1999;17:10-18.
References
- Henderson WLW, Livotti LG, Ford CA, Kelly AB, Lysaght MJ. Clinical experience with intermittent haemodiafiltration. Trans Am Soc Artif Int Organs 19:119-125, 1973
- Petitclerc Th, Devilliers C, Jacobs C. Les pièges du concept de clairance en hémodialyse. Néphrologie 15:273-279, 1994
- Ficheux A, Argilés A, Bosc JY, Mion C. Analysis of the influence of the infusion site on dialyser clearances measured in an " in vitro " system mimicking haemodialysis and haemodiafiltration. Blood Purif 17:10-18, 1999
- Polashegg HD and Levin NW. Hemodialysis machines and monitors. In " Replacement of renal function by dialysis " Fourth edition (Editors Jacobs C, Kjellstrand CM and Koch KM), pages 368-369, 1996
- Polashegg HD. Automatic nonivasive intradialytic clearance measurment. Int J Art Organ 16:185-191, 1993
- Canaud B, Flavier JL, Argilés A, Stec F, NGuyen QV, Bouloux Ch, Garred LJ, Mion C. Hemodiafiltration with on-line production of substitution fluid: Long-term safety and quantitative assessment of efficacy. Contr Nephrol 108:12-22, 1994
- Ahrenhold P, Winkler RE, Ramlow W, Tiess M, Müller W. On-line hemodiafiltration with pre-and post-dilution : a comparison of efficacy. Int J Artif Organs 20 :81-90, 1997
- Ficheux A, Argilés A, Mion C, Mion H. Influence of convection on small molecule clearances. Definition of mathematical laws and their experimental verification in vitro and in vivo. Kidney Int (in press)
- Kerr PG, Argilés A, Flavier JL, Canaud B, Mion C. Comparison of hemodialysis and hemodiafiltration: A long-term longitudinal study. Kidney Int 41:1035-1040, 1992
- Kerr PG, Argilés A, Canaud B, Flavier JL, Mion C. The effects of reprocessing high-flux polysulfone dialysers with peroxyacetic acid on beta 2 microglobulin removal in hemodiafiltration. Am J Kidney Dis 19:433-438, 1992

 Degassed, reverse osmosis, warmed water was used for the blood compartment fluid. Precise QD and QB were checked by collecting the volumes over a time period before and at the end of each series of measurements. Three repeats were performed for each control point.
Degassed, reverse osmosis, warmed water was used for the blood compartment fluid. Precise QD and QB were checked by collecting the volumes over a time period before and at the end of each series of measurements. Three repeats were performed for each control point. QD influence on total ion clearance. Figure 2-b depicts the experiments performed with a range of QD from 420 to 970 ml/min. For a fixed QB = 350 ml/min the total ion clearance increased from 258±5 to 301±1 ml/min (Fig 2-b).
QD influence on total ion clearance. Figure 2-b depicts the experiments performed with a range of QD from 420 to 970 ml/min. For a fixed QB = 350 ml/min the total ion clearance increased from 258±5 to 301±1 ml/min (Fig 2-b).
