PANEL DE DISCUSION |
Tomilina N.A., Androussev A.M., Ermolenko V.M., Melikian A.M., Zentchenko I.V., Volpian L.L., Domakhina A.G.
e-mail: tomilina@glasnet.ru
INTRODUCTION
The treatment of ESRD is still one of the major healthcare issues in Russia. Continuous ambulatory peritoneal dialysis (CAPD) may play a key role in solving this problem.
Lower cost of CAPD compared to HD drives PD penetration in countries with public funding of ESRD treatment programs [5, 10, 13]. However this advantage of CAPD can not be extrapolated on Russia since due to current economic conditions there is no difference between costs of these two modalities in this country. But the advantages of CAPD are not limited to economic ones only. In Russia with its large distances and low density of population CAPD has a particular advantage for the patients who live far from a dialysis center.
CAPD program in Russia was started in January 1995 in Moscow City and Moscow Region with the following opening of PD centers in Saint-Petersburg and other major cities - Ekaterinburg, Novosibirsk, Krasnodar, Khabarovsk, Kazan, Ulyanovsk. But a difficult economic situation is still hampering successful development of this modality so that CAPD patients account for only 5.3% of the overall dialysis population. As a matter of fact CAPD has been significantly developed only in Moscow and Saint-Petersburg where 24% of the overall dialysis population are on CAPD. This article features the results of the biggest CAPD program in Russia - CAPD Moscow program over the period from January 1995 through December 1998. The results of CAPD therapy are compared to those of HD.
SUBJECTS AND METHODS
The information presented in this article is based on the Moscow City ESRD Registry that was created in January 1995.
In 1999 there were 1726 ESRD patients in Moscow with its population of 9 million (191.8 patients per million population). Diabetic patients accounted for 15%, patients over 65 years old - 17.4%. The number of incident patients over the last 4 years has been remaining stable at the level of 530-560 per year, or 60 per million population.
1289 ESRD patients in Moscow were treated with dialysis over the period from January 1st, 1995 through December 31st, 1998. 324 patients (25%) were treated with CAPD and 765 patients - with HD. The age range was 15-85 years with patients of 40-65 years old prevailing; patients over 65 years old accounted for 12%. The HD patients' age range was the same with major portion younger than 55 years; the portion of patients over 65 years old was 12% as well.
The primary renal disease distribution among CAPD and HD patients was approximately the same: diabetic nephropathy 15% and 14%, glomerulonephritis - 43% and 41%, other renal diseases - 42% and 45%, respectively.
In more than 80% of HD patients dialysis was started at the stage of advanced uremia. The percentage of advanced uremia at the onset of CAPD treatment was high as well. By the start of the therapy creatinine clearance (Ccr) over 10 ml/min was in 40% of the patients only while the majority (60%) of the patients had Ccr below 10 ml/min. This late start in many patients was related to the shortage of dialysis spaces.
The treatment outcomes were estimated by mortality rate (percentage of deaths over one calendar year) as well as by patient and technique survival (Kaplan-Meier). Patients who underwent renal transplantation within first 6 months of dialysis were excluded from the calculation of survival rate. When a dialysis modality changed only the initial modality was taken into account.
Peritonitis rate was estimated as the patient-months number per one episode. The peritonitis probability at various times after CAPD initiation was calculated according to Kaplan-Meier. In these calculations all peritonitis episodes including recurrent were taken into account.
The impact of separate factors on the treatment outcomes was analyzed with Cox regression model and with c2 criterion.
RESULTS
The dynamics of CAPD patients count and its portion within overall dialysis population in Moscow is presented at Fig.1. The length of treatment of 41% of the patients exceeded 12 months. In 36% of patients CAPD was performed less than 6 months since CAPD was implemented as a pre-transplant treatment.

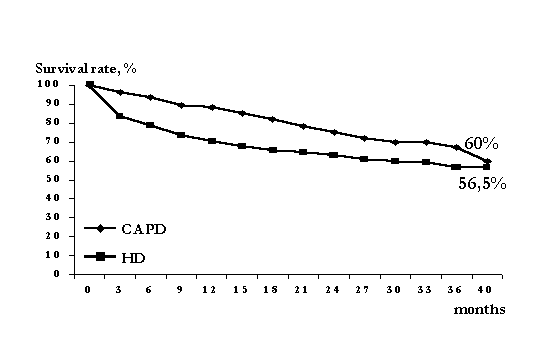
40-months survival did not significantly differed between CAPD and HD patients and was 60% and 56.5%, respectively (Fig.2). Two-year survival in CAPD was slightly higher than in HD. Three-year survival in non-diabetic patients was similar in CAPD (66%, n=275) and HD (60%, n=648) while 30-months survival in diabetic patients was significantly higher in CAPD (69%, 45 patients) than in HD (50%, 119 patients) (?<0,02) (Fig.3).
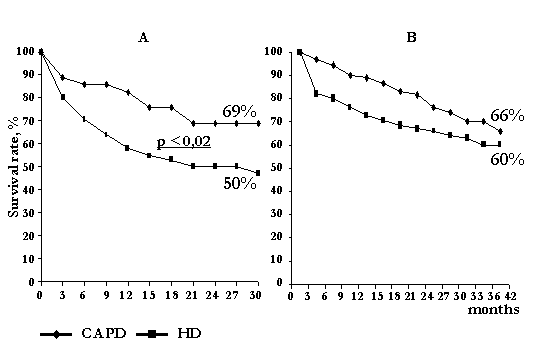
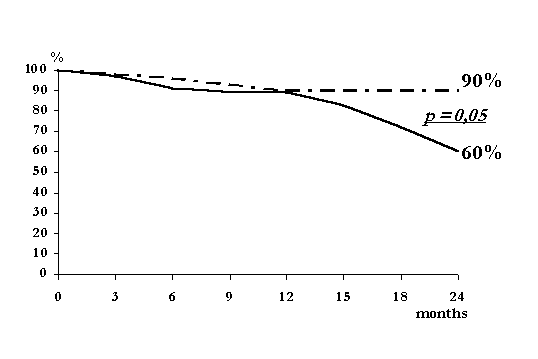
Cox regression analysis showed that factors which have an impact on CAPD outcomes include Kt/V (p<0.001), creatinine clearance (p<0.001) and peritoneal transport characteristics (p<0.001) as well. So survival rate in high transporters was significantly lower than in high-average transporters (Fig.4).
Mortality rate in CAPD was 10.5% of all prevalent patients. Mortality structure was not significantly different between CAPD and HD. The most common cause of death in both groups were cardiovascular diseases (60% and 61%, respectively) while infectious complications as a cause of death were significantly less frequent (14% both in CAPD and HD). However cardiovascular diseases as a cause of death differed in CAPD patients and in HD ones. So congestive heart failure was the most frequent cause of death in HD patients (31%) but it was twice less frequent (16%, p<0.05) in CAPD patients while mortality rate due to stroke was in CAPD patients more frequent (24%).
Three-year technique survival in CAPD was only 53% (Fig.5). Fluid control problems that resulted in overhydration were the most common cause of transfer to HD. Peritonitis as a cause of transfer to HD was less frequent (24%).
Peritonitis rate appeared to be one episode per 19 patient-months. Noteworthy is the fact that peritonitis occurred typically within the first year of treatment (Fig. 6). As shown at the Fig. 6, peritonitis occurred most often within the range from 3 to 9 months, after that period peritonitis rate happened to be stable at the lower level.
Multiple peritonitis episodes made a negative impact on the treatment outcomes (Fig.7). In patients with Kt/V above 1.75 survival rate was significantly lower in the patients who
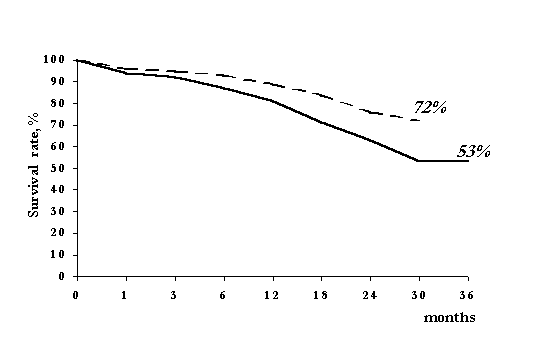
Fig. 5. Three-year CAPD patient and technique survival patient survival technique survival
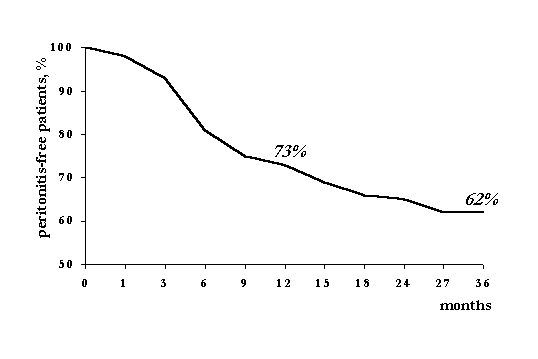
Fig.6. Peritonitis rate probability over time.
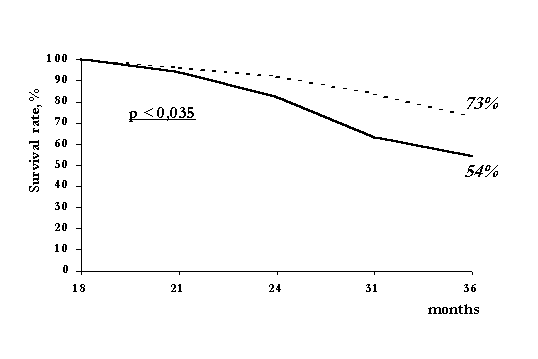
Fig. 7. Impact of multiple peritonitis on CAPD patient survival (CAPD over 18 months) 0-2 peritonitis episodes over 2 peritonitis episodes developed three and more peritonitis episodes when compared to the patients with less than two peritonitis episodes or no peritonitis. However the cause of transfer to HD of patients who developed more than three episodes of peritonitis was typically not peritonitis itself but fluid control problems and cardiovascular complications. Technique failure in patients with multiple peritonitis was 57% while in patients with less than two episodes of peritonitis or no peritonitis it was 17% only (p<0.022).
DISCUSSION
Therefore the efficacy of CAPD and HD in our patients was almost the same and it fully complied with the data from other publications [1, 4, 7, 9, 12]. CAPD appeared to have some advantages for patients with diabetic nephrosclerosis. Three-year patient survival in non-diabetic kidney damage was not different between CAPD and HD (Fig. 3) while 30-months patient survival in diabetic nephropathy was significantly higher in CAPD (Fig. 3). However one should take into account that our HD patients were generally in more advanced state of disease than CAPD ones; thus our data can not prove a higher efficacy of CAPD in diabetic nephropathy.
Like some other authors [4] we observed higher two-year patient survival in CAPD compared to HD. Although this data needs further clarification we suppose that it demonstrates CAPD feasibility prior to kidney transplantation. This approach enables to significantly increase the availability of renal replacement therapy under the circumstances of HD shortage. Our CAPD population included a particularly high number of patients with markedly decreased renal function and severe overall clinical condition prior to initiation of treatment. This may have had a negative impact on the treatment outcomes. Noteworthy is the fact that peritonitis episodes in our patients occurred most frequently within the first year of treatment although bacterial contamination was expected to be more probable along with the increase of treatment length.
Patients with multiple peritonitis appeared to more frequently develop overhydration and cardiac failure that required transfer to HD. It is obvious that these complications were the result of inadequate ultrafiltration caused by disorders of peritoneal permeability to low-molecular solutes [2, 6, 11]. The interrelation between peritonitis and subsequent peritoneal loss of ultrafiltration is being discussed in literature [6, 8]. Some authors prove that this interrelation exists at least for peritonitis occurred within first 18 months of treatment while other authors deny this interrelation. Our data complies with the results of Davies et al [3], as well as with data from Kawagushi, 1999 [8] who observed higher patient survival rate in the centers with significantly lower peritonitis incidence.
Although we did not focus special attention on the dynamics of peritoneal transport characteristics and ultrafiltration capabilities in our patients, their high and stable Kt/V values allow us to exclude the possibility of decreased peritoneal dialyzing surface due to sclerosis. We deem very likely that multiple peritonitis episodes result in the damage to peritoneal membrane structure, which lead to inadequate ultrafiltration and consequent overhydration.
We consider CAPD in Russia a very perspective RRT option that has the same with HD efficacy. Even though CAPD does not seem to have economic advantages over HD it is still very important for the regions with big territories and low density of population. The importance of this modality in Russia is high since it enables as well to optimize the issue of RRT availability for the potential allograft recipients. Peritonitis in our patients proved to be a major issue since their high incidence is a factor increasing technique failure probability.
REFERENCES