
R.Solà MD.
| DISCUSSION BOARD |
At the same time, due to the aging of the general population, dialysis programs now include more elderly people and the demand for transplantation has consequently also risen in this group of patients.
As a result of this increase in both elderly donors and elderly recipients, different strategies have been proposed for the utilization of suboptimal kidneys. Some authors support the use of a double transplant with this type of donor and report better allograft function when a greater renal mass is transplanted, However, survival of graft and patient at two-year follow-up shows no significant differences in respect to single transplants from the same type of donor. Although the creatinine clearance values in recipients of single suboptimal grafts are higher than in recipients of a double graft, these levels do not appear to worsen during follow up. In other words, double transplant may be more efficacious because it achieves a better allograft function but it does not appear to be more efficient as it unnecessarily reduces the number of patients who may receive transplantation.
Other authors believe suboptimal kidneys should be reserved for elderly patients on the grounds that although the smaller kidney mass in such grafts may diminish further in time due to ischemia-reperfusion lesions, acute rejection, toxicity of some immuno-depressors and certain infectious processes. the metabolic demand in this population group is also lower.
However, such matching has been associated with a greater morbi-mortality in comparison with transplants from younger donor kidneys. In our series of 120 elderly kidney recipients we observed significant differences in graft and patient survival at five years depending on whether the graft was suboptimal or from a younger donor (85% and 54% vs 91% and 65% respectively, p<0.0005).
Nevertheless, the main cause of graft loss in both groups was patient exitus. This would suggest that although a suboptimal kidney clearly plays a significant role, patient death is mainly due to the recipient age, In various studies it has also been observed that patient survival is influenced by receptor age, whereas donor age is only reflected post-transplantation in higher creatinine clearance values, and these do not worsen over time.
Such findings suggest that kidneys from suboptimal donors are valid for transplant but may be better matched to younger recipients.
Aware that the renal mass is sufficient but somewhat limited, we attempted to match suboptimal kidneys with younger donors of the same sex with a similar body mass index. A total of 63 kidney grafts from donors over 60 years of age (median age 67.1+6.6 years) were transplanted to recipients under 60 years of age (median age 5.6+8.3 years) and results compared with a control group of 235 patients transplanted over the same period but in whom both donor and recipient age was below 60 (34.3+15.2+40.6+12.6 years respectively).
Annual serum creatinine remained stable during the study period although the levels were higher in the study group as compared to the control group. Also in the first group, donor age, female donor/male recipient match and acute rejection alone or together with acute tubular necrosis were determinants for worse allograft function at one year depending on whether serum creatinine was above or below 150mol/l. Of the 43 grafts with a minimal follow up of two years in this group, renal function remained stable in 36. Chronic allograft nephropathy however, which leads to a progressive decrease in renal function, was diagnosed in 9 patients. We were unable to relate this to any specific clinical parameter although a tendency was observed in patients presenting acute rejection and/or acute tubular necrosis, with less diuresis post-graft and a greater number of dialysis sessions due to delayed graft function.
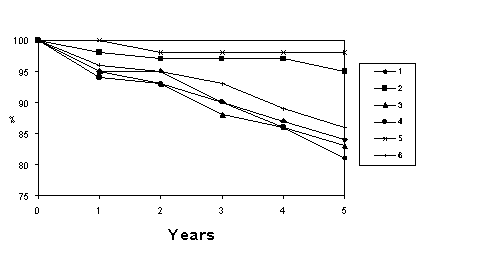
Patient survival at 1 and 5 years was significantly higher in the control group (95% and 84% vs 98% and 95%, respectively). There were no differences regarding graft survival (95% and 83% vs 94% and 81%, respectively), although this was favorable for the first group concerning censored death (100% and 98% vs 96% and 86% in the control group, 9=0.04).
The long-term stability of renal function endorses the suitability of the renal mass transplanted in the former group. Although stable at one year, the risk to present worse renal functioning was related to donor age, female donor/male recipient matching due to the scarce nephron units, and acute tubular necrosis and acute rejectio. Nevertheless, although these lesions may decrease graft function, they are not sufficient to cause chronic allograft nephropathy in younger recipients, probably as there remains a sufficient number of nephron units. The presence and severity of acute tubular necrosis and acute rejection appear to play a more important role.
The highest cause of graft loss was patient exitus. With censured death, graft survival was significantly higher in the first group, which again justifies this type of graft (graph). Whether or not our findings and those of other authors are confirmed in future studies, it seems clear that a better survival at one year post-transplant can be achieved than that cited in the UNOS registery of 93,934 transplants in the United States (95% vs 87.7%).
In conclusion, correct physiological maintenance of the suboptimal donor provides a renal mass which, when protected from posterior lesions during the transplantation process, provides an acceptable renal function that does not deteriorate over time, and which may provide many younger patients with the chance for a good quality of life.