|
Discussion Board
Paneles de Discussión
Paneais de Discussio
Free Papers
Comunicaciones libres
Comunicaçoes livres
Home cin2003
Volver al Inicio cin2003
Voltar ao inicio cin2003
|
The Use of Vitamin C as an Adjuvant Therapy to Recombinant Human Erythropoietin in Patients with End-Stage Renal Disease
Sehsuvar Ertürk, M.D.
Department of Nephrology, Ankara University Medical School.
Ankara, Turkey
erturk@medicine.ankara.edu.tr
Introduction:
Research over the last 25 years has resulted in a favoring of the concept of insufficient synthesis and secretion of erythropoietin as a major cause of anemia of chronic kidney disease.1 Indeed, recombinant human erythropoietin (rhEPO) has revolutionized the management of anemia in patients with end-stage renal disease (ESRD).1-4 However, there is wide variability in effective doses of rhEPO and there are even many reports of resistance to rhEPO.1 The common causes for inadequate response to rhEPO are iron deficiency, inflammation, malnutrition, hyperparathyroidism, aluminum intoxication, and deficiency of vitamin B12 or folate.5-9 After the exclusion of these common factors, other probable causes including genetic factors, use of ACE inhibitors, malignancy, and vitamin C-deficiency should also be considered.9-13
Recently, several studies have searched for adjuvant therapies to rhEPO to provide greater clinical benefits and to make this treatment more cost-effective13-20 The current article focuses on the rationale, benefits, and the limitations of the use of vitamin C in the management of anemia in patients with ESRD.
Rationale
Vitamin C status in ESRD Patients
Chronic hemodialysis patients generally have lower plasma vitamin C levels than healthy subjects,21 possibly caused by the loss of vitamin C during dialysis, increased consumption, or inadequate dietary intake.22,23 It was reported that 1,000 to 1,500 mg/week or 150 to 200 mg/d of vitamin C could normalize the plasma levels in the majority of patients. More recently, Mydlik et al24 reported that 60 mg/d vitamin C replacement prevented vitamin C deficiency in hemodialysis patients without leading to further increase of plasma oxalate levels.
Probable Mechanisms for a Better Response to rhEPO
Beneficial effects of vitamin C in the management of anemia have been reported not only in vitamin C-deficient patients, but also in patients with normal baseline vitamin levels.25 Furthermore, plasma vitamin levels have been reported to rise in a similar manner in both responsive and non-responsive patients.26 Therefore, mechanisms other than the correction of vitamin C-deficiency state should be considered. Although not definitely proven, the probable mechanisms may be related to anti-oxidant properties of vitamin C, and to its effects on iron metabolism or endogenous erythropoietin synthesis. Since vitamin C is one of the most important antioxidants existing in plasma, another possible mechanism for a better response to rhEPO may be increased erythrocyte lifespan via both the prevention of hemoglobin denaturation and erythrocyte membrane lipid peroxidation27,28 Vitamin C increases intestinal iron absorption and induces iron mobilization from inert tissue stores, including reticuloendothelial system, and may improve iron availability. It has also a role in the enzymatic incorporation of iron into protophorphyrin for heme synthesis.29-31. In addition, most intervention studies found a rise of transferrin saturation and/or a decrease in ferritin level in response to vitamin C.19,20,26,32It has been suggested, therefore, that beneficial effect of vitamin C is related to its effects on iron metabolism. Finally, vitamin C, when administrated with the antioxidant vitamins A and E, was shown to lead to an increase in erythropoietin production of isolated serum-free perfused rat kidneys.33 However, this effect was suggested to be a consequence of the protection of cells from oxidative damage as vitamin C alone did not increase erythropoietin production in hepatoma cell cultures.
Clinical Studies
In a small pioneer study, Gastaldello et al.25 showed the beneficial effect of intravenous vitamin C in four iron-overloaded hemodialysis patients, whereas no effect on hematocrit was achieved in seven patients with normal iron status. In that study, dose of intravenous vitamin C was defined as 1,000 mg/wk and study duration was three months. Tarng and Huang reported a significant increase in hematocrit levels together with a 20% reduction in rhEPO dose under 8-week duration of 300 mg thrice-weekly intravenous vitamin C.34 In both studies, beneficial effects of vitamin C paralleled a significant rise in transferrin saturation.
In another study, Tarng et al. administrated 300 mg of vitamin C intravenously after each hemodialysis session for 8 weeks in 37 hyperferritinemic patients (i.e., ferritin > 500 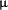 g/L).26 They found the response rate was approximately 50%, and the predictors of the response were transferrin saturation < 25% and erythrocyte zinc protophorphyrin > 105 g/L).26 They found the response rate was approximately 50%, and the predictors of the response were transferrin saturation < 25% and erythrocyte zinc protophorphyrin > 105 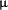 mol/mol heme (indicating insufficient iron incorporation into heme). mol/mol heme (indicating insufficient iron incorporation into heme).
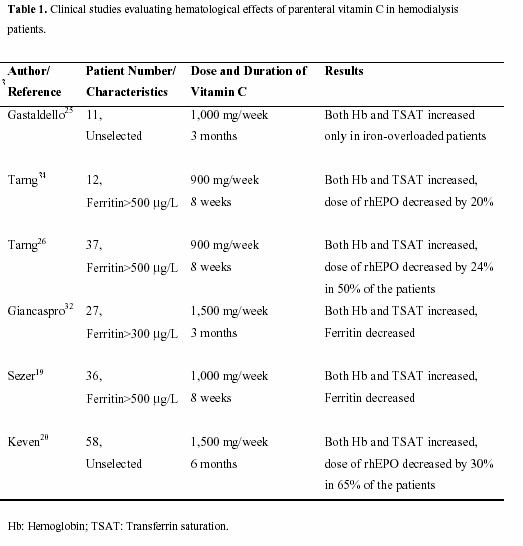
In a prospective, randomized, crossover study, Giancaspro et al. evaluated 27 hemodialysis patients with functional iron deficiency.32 They found that all the patients administrated 500 mg of intravenous vitamin C three times a week for 3 months had significant increases in both hemoglobin and transferrin saturation. The authors also reported that both hemoglobin and transferrin saturation declined after cessation of vitamin C therapy. Sezer et al.19 also reported a significant increase in hemoglobin and decrease in dose of rhEPO in 36 hemodialysis patients whose ferritin level > 500 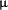 g/L with an 8-week duration of 1g/wk vitamin C treatment. More recently, in a prospective, randomized, crossover study, our group demonstrated that approximately 65% of hemodialysis patients responded to 6-month duration of 1,500 mg/wk of intravenous vitamin C treatment with almost a 2-g/dL increase in hemoglobin level, together with a 2,500-IU/wk (30%) reduction in EPO dose.20 Interestingly, the number of responder patients, increase in hemoglobin levels, and decrease in EPO doses were not different in patients with a ferritin level greater or less than 800 g/L with an 8-week duration of 1g/wk vitamin C treatment. More recently, in a prospective, randomized, crossover study, our group demonstrated that approximately 65% of hemodialysis patients responded to 6-month duration of 1,500 mg/wk of intravenous vitamin C treatment with almost a 2-g/dL increase in hemoglobin level, together with a 2,500-IU/wk (30%) reduction in EPO dose.20 Interestingly, the number of responder patients, increase in hemoglobin levels, and decrease in EPO doses were not different in patients with a ferritin level greater or less than 800 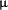 g/L. The clinical studies on the effects of parenteral vitamin C in hemodialysis patients are summarized in Table 1. Finally, a four-week duration of low-dose oral vitamin C treatment was also shown to lead to a significant increase in hemoglobin in hemodialysis patients24 g/L. The clinical studies on the effects of parenteral vitamin C in hemodialysis patients are summarized in Table 1. Finally, a four-week duration of low-dose oral vitamin C treatment was also shown to lead to a significant increase in hemoglobin in hemodialysis patients24
 Limitations
Long-term high doses of vitamin C treatment might be a potential risk for the development of secondary oxalosis in ESRD patients. Shah et al35 reported 19% increase in plasma oxalate levels after 4 weeks of 100 m/d oral vitamin C in peritoneal dialysis patients. Ono also found high oxalate levels after 500 mg/d of oral vitamin C supplementation of longer than 6 months, and suggested that hyperoxalemia is aggravated by long duration of vitamin C supplementation in hemodialysis patients.36 Although plasma oxalate levels were not assessed in many interventional studies mentioned above, Tarng et al.26 showed no significant increase in oxalate levels with intravenous vitamin C treatment of 300 mg thrice weekly. Nevertheless, caution is warranted when using long-term vitamin C treatment in hemodialysis patients.
Another probable limitation for the use of vitamin C to achieve a better anemia control in hemodialysis patients is the lack of any proven mechanisms for the beneficial effects. It is also unclear whether it is related to baseline plasma vitamin C levels. Furthermore, there is currently no consensus on the use of vitamin C in patients with normal iron status.
Conclusion
After the exclusion of the common causes of hypo-responsiveness, intravenous vitamin C replacement may be used as an adjuvant therapy to rhEPO in hemodialysis patients, particularly in those with functional iron deficiency. Future larger-sized interventional studies, however, are needed to prove its safety and to find out the mechanisms of its beneficial effects.
References:
- Eschbach JW, Varma A, Stivelman JC: Is it time for a paradigm shift? Is erythropoietin deficiency still the main cause of renal anemia? Nephrol Dial Transplant 17 (Suppl 5):2-7, 2002.
- Eschbach JW: The anemia of chronic renal failure: Pathophysiology and the effects of recombinant erythropoietin. Kidney Int 35:134-148, 1989.
- Winearls CG, Oliver DO, Pippard MJ, Reid C, Downing MR, Cotes PM: Effect of human erythropoietin derived from recombinant DNA on the anemia of patients maintained by chronic hemodialysis. Lancet 2:1175-1178, 1986.
- Eschbach JW, Egrie JC, Downing MR, Browne JK, Adamson JW: Correction of the anemia of end-stage renal disease with recombinant human erythropoietin: Results of a combined phase I and II clinical trial. N Engl J Med 316:73-78, 1987.
- Adamson JW, Eschbach JW: Management of the anemia of chronic renal failure with recombinant human erythropoietin. Q J Med New Series 73:1093-1101, 1989.
- Kaiser L, Schwartz KA: Aluminum induced anemia. Am J Kidney Dis 6:348-352, 1985.
- Potasman I, Better OS: The role of secondary hyperparathyroidism in the anemia of chronic renal failure. Nephron 33:229-231, 1983.
- Hampers CL, Streiff R, Nathan DG, Snyder D, Merrill JP: Megaloblastic hematopoiesis in uremia and in patients on long-term hemodialysis. N Engl J Med 276:551-554, 1967.
- National Kidney Foundation: K/DOQI Clinical Practice Guidelines for Anemia of Chronic Kidney Disease, 2000.Am J Kidney Dis 37 (Suppl 1):S182-S238, 2001.
- Ertürk S, Kutlay S, Karabulut HG, et al: The impact of vitamin D receptor genotype on the management of anemia in hemodialysis patients. Am J Kidney Dis 40:816-823, 2002.
- Ertürk S, Ates K, Duman N, Karatan O, Erbay B, Ertug E: Unresponsiveness to recombinant human erythropoietin in haemodialysis patients: Possible implications of angiotensin-converting enzyme inhibitors. Nephrol Dial Tranplant 11: 396-397, 1996.
- Ertürk S, Nergizoglu G, Ates K, et al: The impact of withdrawing ACE inhibitors on erythropoietin responsiveness and left ventricular hypertrophy in haemodialysis patients. Nephrol Dial Transplant 14: 1912-1916, 1999.
- Hörl WH: Is there a role for adjuvant therapy in patients being treated with epoetin? Nephrol Dial Transplant 14 (Suppl 2):S50-S60, 1999.
- Labonia WD: L-Carnitine effects on anemia in hemodialyzed patients treated with erythropoietin. Am J Kidney Dis 26:757-764, 1995.
- Kooistra MP, Struyvenberg A, van Es A: The response to recombinant human erythropoietin in patients with the anemia of end-stage renal disease is correlated with serum carnitine levels. Nephron 57:127-128, 1991.
- Berard E, Iordache A: Effects of low doses of Lcarnitine on the response to recombinant human erythropoietin in hemodialyzed children: About two cases. Nephron 62:368-369, 1992.
- Berns JS, Rudnick MR, Cohen RM: A controlled trial of recombinant human erythropoietin and nandrolone decanoate in the treatment of anemia in patients on chronic hemodialysis. Clin Nephrol 37:264-267, 1992.
- Ballal SH, Domato DT, Polack DC, Marciulonis P, Martin KJ: Androgens potentiate the effects of erythropoietin in the treatment of anemia of end-stage renal disease. Am J Kidney Dis 17:29-33, 1991.
- Sezer S, Ozdemir FN, Yakupoglu U, Arat Z, Turan M, Haberal M: Intravenous ascorbic acid administration for erythropoietin-hyporesponsive anemia in iron overloaded hemodialysis patients. Artif Organs 26:366-370, 2002.
- Keven K, Kutlay S, Nergizoglu G, Ertürk S: Randomized, crossover study of the effect of vitamin C on EPO response in hemodialysis patients. Am J Kidney Dis 41:1233-1239, 2003.
- Descombes E, Hanck AB, Fellay G: Water soluble vitamins in chronic hemodialysis patients and need for supplementation. Kidney Int 43:1319-1328, 1993.
- Sullivan JF, Eisenstein AB: Ascorbic acid depletion in patients undergoing chronic hemodialysis. Am J Clin Nutr 23:1339-1346, 1970.
- Pönka A, Kuhlback B: Serum ascorbic acid in patients undergoing chronic hemodialysis. Acta Med Scand 213:305-307, 1983.
- Mydlik M, Derzsiova K, Boldizsar J, Hribikova M, Petrovicova J: Oral use of iron with vitamin C in hemodialyzed patients. J Ren Nutr 13:47-51, 2003.
- Gastaldello K, Vereerstraeten A, Nzame Nze T, Vanherweghem L, Tielemans C: Resistance to erythropoietin in iron overloaded hemodialysis patients can be overcome by ascorbic acid administration. Nephrol Dial Transplant 10 (Suppl 6):S44-S47, 1995.
- Tarng DC,Wei YH, Huang TP, Kuo BIT: Intravenous ascorbic acid as an adjuvant therapy for recombinant erythropoietin in hemodialysis patients with hyperferritinemia. Kidney Int 55:2477-2486, 1999.
- Rosenmund A, Binswanger U, Straub PW: Oxidative injury to eryhrocytes, cell rigidity, and splenic hemolysis in hemodialyzed uremic patients. Ann Intern Med 82:460-465, 1975.
- Candan F, Gültekin F, Candan F: Effect of vitamin C and zinc on osmotic fragility and lipid peroxidation in zinc-deficient haemodialysis patients. Cell Biochem Funct 20:95-98, 2002.
- Banerjee S, Chakrabarty AS: Utilization of iron by scorbutic guinea pigs. Blood 25:839-844, 1965.
- Bridges KR, Hoffman KE: The effects of ascorbic acid on the intracellular metabolism of iron and ferritin. J Biol Chem 261:14273-14277, 1986.
- Lipschitz DA, Bothwell TH, Seftel HC,Wapnick AA, Charlton RW: The role of ascorbic acid in the metabolism of storage iron. Br J Haematol 20:155-163, 1971.
- Giancaspro V, Nuzziello M, Pallotta G, Sacchetti A, Petrarulo F: Intravenous ascorbic acid in hemodialysis patients with functional iron deficiency: A clinical trial. J Nephrol 13:444-449, 2000.
- Jelkmann W, Pagel H, Hellwig T, Fandrey J: Effects of antioxidant vitamins on renal and hepatic erythropoietin production. Kidney Int 51:497-501, 1997.
- Tarng DC, Huang TP: A parallel, comparative study of intravenous iron versus intravenous ascorbic acid for erythropoietin hyporesponsive anemia in hemodialysis patients with iron overload. Nephrol Dial Transplant 13:2867-2872, 1998.
- Shah GM, Ross EA, Sabo A, Pichon M, Bhagavan H, Reynolds RD: Ascorbic acid supplements in patients receiving chronic peritoneal dialysis. Am J Kidney Dis 18:84-90, 1991.
- Ono K: Secondary hyperoxalemia caused by vitamin C supplementation in regular hemodialysis patients. Clin Nephrol 26: 239-243, 1986.
|
