
|
Paneles de Discussión
Paneais de Discussio |
The association between pre-transplant C-reactive protein and chronic allograft nephropathy in renal transplant recipients highlights the importance of atherogenesis in this diseaseJeffrey C. Fink MD, MSDivision of Nephrology, Department of Medicine, University of Maryland School of Medicine, Baltimore. USAJfink@medicine.umaryland.eduChronic allograft nephropathy (CAN), also known as chronic rejection, has been a major cause of allograft failure in renal transplant recipients ranking only second after death with a functioning allograft . Despite major improvements in short term allograft survival rates, CAN continues to limit transplant survival in a large portion of this population [1,2]. Several pathogenic factors, are likely to contribute to the development of CAN and these can be divided into alloantigen-dependent and alloantigen-independent processes[3].
The primary alloantigen-dependent event associated with CAN is acute rejection, which is a strong risk factor for development of CAN and accelerated allograft loss [4]. Several allogenic-independent factors have been invoked as important in the development of CAN such as chronic exposure to calcineurin inhibitors, diminished nephron dose at transplant, and preservation injury [3]. One factor that is likely to be important in the development of CAN is artherosclerosis, which is likely to contribute to the transplant vasculopathy of CAN [5,6]. In renal transplantation, accerelerated atherogenesis is considered to be an important risk factor for transplant vasculopathy for several reasons[7]. Many of the pathologic vascular characteristics of CAN are analogous to those seen in systemic vascular atherosclerotic lesions with macrophages and lymphocytes along with lipoprotein deposits[8,9]. The vasculopathy found in the CAN of renal transplant patients is strikingly similar to the coronary vascular lesions found in the chronic rejection of cardiac transplant patients [6,10]. Furthermore, hyperlipidemia appears to be a risk factor for development of CAN in renal transplant recipients [11,12]. Observational studies have demonstrated an association between inflammation, as reflected by elevations of CRP and sICAM-1, and subsequent development of clinically significant CVD in both the general population and patients with ESRD [13-17]. The interaction between inflammation and atherosclerosis hypothesized as the putative process leading to CVD in the general population may also induce the manifestations of ASCVD in the renal transplantation population, which includes CAN. ASCVD is likely to be an important factor in premature allograft loss in renal transplant patients both by contributing to the pathogenesis of CAN and leading to death from CVD. Therefore, it is quite possible that pre-transplant elevations of inflammatory markers are associated with CAN after renal transplantation. To demonstrate this association between the inflammatory marker, CRP and CAN, a case-control study was conducted comparing pre-transplant CRP concentrations in transplant recipients with confirmed CAN to CRP levels in a stable control group [18]. The controls were renal transplant patients who received their allograft during the same period as the cases with stable renal function and no need for a transplant biopsy for allograft dysfunction. The results are shown in Fig 1. 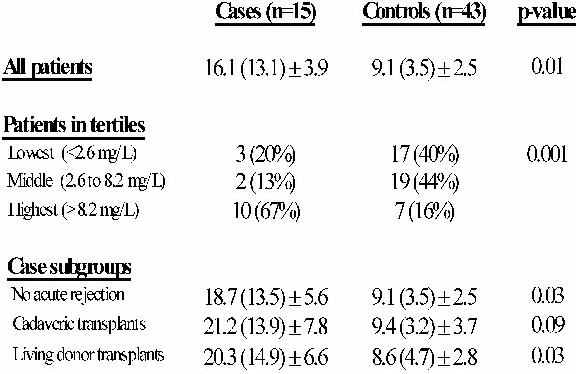
Figure 1 Mean (median) pre-transplant C-reactive protein concentration (mg/L) in renal transplant recipients with chronic allograft nephropathy (cases) versus controls [18]
The association between CRP and CAN underscores the likelihood of a common pathogenesis between atherogenesis and CAN in renal transplantation. The results suggest that pre-transplant inflammatory markers can be used to stratify individuals into risk groups for CAN and would allow providers to customize immunosuppressive regimens to minimize the likelihood of this outcome. This association also emphasizes the critical importance of intervening on several modifiable cardiovascular risk factors such as smoking, hyperlipidemia, hypertension and glucose intolerance, which lead to the ASCVD in the transplant population.
References 1. Gjertson DW: Survival trends in long-term first cadaveric donor kidney transplants; in: Terasaki PI (ed): Clinical Tranplantation 1991. Los Angeles, UCLA Tissue Typing Laboratory p 225. 2. Paul LC, Benediktsson H: Chronic transplant rejection. Transplant Reviews 1993;7:96-113. 3. Tullius SG, Tilney NL: Both alloantigen-dependent and independent factors influence chronic allograft rejection. Transplantation 1995;59:313-318. 4. Kahan BD: Toward a rational design of clinical trials of immunosuppressive agents in transplantation. Immunol Review 1993;136:29-49. 5. Ludwig J, Wiesner RH, Batts KP, Perkins JD, Krom RA: The acute vanishing bile duct syndrome (acute irreversible rejection) after orthotopic liver transplantation. Hepatology 1987;7:476-483. 6. Kobashigawa JA, Katznelson SA, Laks H, Johnson JA, Yeatman L, Wang XM, Chia D, Terasaki PI, Sabad A, Cogert GA, Trosian K, Hamilton MA, Moriguchi JD, Kawata N, Hage A, Drinkwater DC, Stevenson LW: Effect of pravastatin on outcomes after cardiac transplantation. N Engl J Med 1995;333:621-627. 7. Kasiske BL: Role of circulating lipid abnormalities in chronic renal allograft rejection. Kidney Int 1999;71 (Supplement):S28-S30. 8. Hume DM, Merrill JP, Miller BF, Thorn GW: Experiences with renal homotransplantation in the human: report of nine cases. J Clin Invest 1955;24:327-382. 9. Paul LC, Fellstrom B: Chronic vascular rejection of the heart and the kidney--have rational treatment options emerged? Transplantation 1992;53:1169-1179. 10. Alonso DR, Starek PK, Minick CR: Studies on the pathogenesis of atheroarterosclerosis induced in rabbit cardiac allografts by the synergy of graft rejection and hypercholesterolemia. Am J Pathol 1977;87:415-442. 11. Isoniemi H, Nurminen M, Tikkanen M, Von Willebrand E, Krogerus L, Ahonen J, Ecklund B, Hockerstedt K, Salmela K, Hayry P: Risk factors predicting chronic rejection of renal allografts. Transplantation 1994;57:68-72. 12. Guijarro C, Massy ZA, Kasiske BL: Clinical correlation between renal allograft failure and hyperlipidemia. Kidney Int 1995;52 (Supplement):S56-S59. 13. Ridker PM, Stampfer MJ, Rifai N: Novel risk factors for systemic atherosclerosis: A comparison of C-reactive protein, fibrinogen, homocysteine, lipoprotein (a), and standard cholesterol screening as predictors of peripheral vascular disease. JAMA 285:2481-2485, 2001 14. Ridker PM, Hennekens CH, Rotman-Johnson B, Stampfer MJ, Allen J: Plasma concentration of soluble intercellular adhesion molecule 1 and risks of future myocardial infarction in apparently healthy men. Lancet 351:88-92, 1998 15. Ridker PM, Hennekens CH, Buring JE, Rifai N: C-reactive protein and other markers of inflammation in the prediction of cardiovascular disease in women. N Engl J Med 342:836-843, 2000 16. Iseki K, Tozawa M, Yoshi M, Fukiyama K: Serum C-reactive protein (CRP) and risk of death in chronic dialysis patients. Nephrol Dial Transplant 14:1956-1960, 1999 17. Yeun JY, Levine RA, Mantadilok V, Kaysen GA: C-reactive protein predicts all-cause and cardiovascular mortality in hemodialysis patients. Am J Kidney Dis 35:469-476, 2000 18. Fink JC, Onuigbo MA, Blahut SA, Christenson RH, Mann D, Bartlett ST, Weir MR: Pre-transplant serum C-reactive protein and the risk of chronic allograft nephropathy in renal transplant recipients: a pilot case-control study. Am J Kidney Dis 39:1096-1101, 2002 |