
|
Paneles de Discussión
Paneais de Discussio |
ALTRUISTIC LIVING DONORS: EXPLORING THE OPTION Reginald Y. Gohh, MD, Assistant Professor of Medicine
Division of Organ Transplantation, Rhode Island Hospital Brown University School of Medicine Providence, RI. USA INTRODUCTION The success of kidney transplantation has created an unprecedented demand for a limited supply of kidney donors. Despite aggressive public service and media efforts to increase the rate of cadaver organ donation, it is evident that the annual number of available deceased organ donors will never be sufficient to meet the demands of the ongoing organ shortage. Currently over 55,000 patients are registered on the national waiting list for a renal transplant and median waiting times now exceed three years in much of the country1. Additionally, recent data have demonstrated the importance of time spent on dialysis as a mortality risk factor, thus stressing the importance of exploring all possible options for transplantation2. To address this problem, the majority of transplant centers have relied on living donors as an important kidney source and nationally, living donors now provide 42% of all kidney transplants1. Kidneys from live donors provide superior results to cadaver sources, regardless of the genetic relationship to the recipient3-6. Furthermore, long-term data have demonstrated the relative safety of the living-donor operation, showing no impact on either longevity or quality of life7-9. Thus, the current standard adopted by most transplant centers is to consider any adult as an organ donor who is motivated, competent, free of coercion, and medically and psychologically fit. Traditionally, these individuals have been intimately related to the identified recipient, either genetically or through an emotional bond. From time to time, transplant centers and organ procurement organizations across the country receive inquiries from individuals seeking to donate a kidney to a stranger in need of a transplant. The typical response of the transplant center to these "good Samaritan donors" is a gracious acknowledgement of the offer, but to nonetheless dismiss the request because of a lack of relationship between donor and recipient. However, the success of kidney transplantation from a genetically unrelated living spouse or friend and the compelling need to provide for an ever-expanding waiting list have influenced transplant physicians to at least consider the requests of such individuals. We have accepted altruistic donors since one unsolicited offer to our group in 1999. The following describes our strategy in handling such requests. The psychological and emotional impact of donation on these altruistic donors has received little attention thus far.. Herein, we provide follow-up of individuals whose requests for altruistic donation were ultimately approved. METHODS Since 1999, 160 kidney transplants from living donors were performed at Rhode Island Hospital. Of these, seven fit the description of an altruistic donor. These volunteers met at least one of the following criteria: 1 they either expressed a desire to donate a kidney to any suitable recipient on our waiting list that he or she did not know or2 were aware of a particular individual in need of an organ transplant (e.g. through public or media appeals) but had no relationship with that recipient. Our efforts to recruit such volunteers were unsolicited, and relied upon the potential altruistic donor to initiate contact. A comprehensive information packet regarding the practice of living donation, including inclusion and exclusion criteria was mailed to all potential donors. If the potential donor initiated further contact, an initial screening interview was scheduled with a trained transplant coordinator. The objectives of the interview were to discuss in detail the donation process (including the pre-operative evaluation, the operation and associated risks, recovery time, potential long-term complications, and potential donor costs). The meeting also provided an opportunity to evaluate for the presence of medical and social contraindications to surgery and to evaluate the donor’s motivation and ability to give an informed consent. Satisfactory completion of the initial screening resulted in the donor being referred for medical and surgical evaluation by a transplant physician and surgeon respectively. In this regard, the criteria for medical suitability for kidney donation made no distinction between the altruistic and the emotionally/genetically-related donor, since the risks of surgery are independent of these relationships. However, increased emphasis was placed on the psychosocial evaluation of Good Samaritan donors. As opposed to related donors where the obvious rationale to donation is to improve the health of a person with whom they share a relationship, no such well-defined benefit can be ascribed to the altruistic donor. Such donor requests were referred for comprehensive psychiatric evaluation to ensure that the motives for donating were acceptable and realistic and to exclude underlying major psychiatric illness. Kidneys were allocated to patients on our transplant center’s waiting list based on the recipient waiting time and human leukocyte antigen (HLA) matching. Hypothetically, altruistic donors would have been offered the opportunity to donate to potential 0-mismatch recipients anywhere within our organ procurement region if such individuals were identified. Our center felt comfortable employing this allocation system since it provided an unbiased and objective means to identifying prospective recipients. Although potential donors were given an opportunity to express a preference of recipients (e.g. children, disadvantaged minorities), all agreed to adhere to the aforementioned protocol for selecting recipient patients. Once the recipient was identified, both donor and recipient were given an opportunity to communicate before the transplant, if both parties so desired. Given the enormous sacrifice that the Good Samaritan donor was about to endure, we felt that it was within their right to request such a meeting. Furthermore, such correspondence could provide a tangible bond to the recipient, which is inherently not the case in altruistic donation. In our series, only one individual who volunteered as a non-directed donor wished to remain anonymous to the fortunate recipient of her good will. Finally, although the long-term psychological benefits of being a directed donor are well established, the consequences to altruistic donors are not. Based on our single-center experience, we distributed quality-of-life studies and psychological assessments to all Good Samaritan donors in our program to examine their thoughts on this important issue. The group was administered a health-related quality-of-life survey (SF-12) in addition to questions designed by the authors to review their experiences and present attitudes towards altruistic donation. The surveys were answered and returned anonymously. The entire cohort responded to our queries. RESULTS The characteristics of the seven altruistic donors in our program are shown on Table I. These include three individuals who volunteered as non-directed donors and four who donated to a particular patient with whom they had no previous relationship. The average age of the donors was 46 years; all were Caucasians with the overwhelming majority being female. The group as a whole was well educated with seven of eight patients receiving education beyond the high school level. Of note, all individuals were employed on a full-time basis. Table 1. Demographic characteristics of altruistic living donors
* Denotes Caucasian race The mean follow-up since transplant was 633 days. All donors judged themselves to be in excellent health. None felt that their lifestyles were limited physically because of donor nephrectomy (2 laparoscopic, 5 open). No patients complained of residual pain that compromised their work both outside and inside their household. None reported any emotional problems that impacted on their social activities and all participants gauged their state of mind to be calm and peaceful at least most of the time. Regarding their experiences as an organ donor, all expressed extreme satisfaction from donating and none regretted their decisions. If placed under similar circumstances, not only did all participants confirm that they would donate a kidney again, but the majority would also recommend donation if asked by another person. With the exception of one individual, all donors stated that families and friends were strongly supportive of their decision to donate a kidney. The majority (5/7) felt that they derived as much satisfaction from donating a kidney to a stranger as if the recipient had been a close friend or relative, whereas two individuals were ambivalent about the issue. Finally, all altruistic donors expressed satisfaction regarding the handling of their living donation and the information received from our transplant program. However, one donor did express regret in meeting her recipient due to some later disappointing interactions with that person. Figure 2. Mini-laparotomy donor nephrectomy: in the open procedure the kidney is removed from a 3.5 inch anterior retroperitoneal approach.
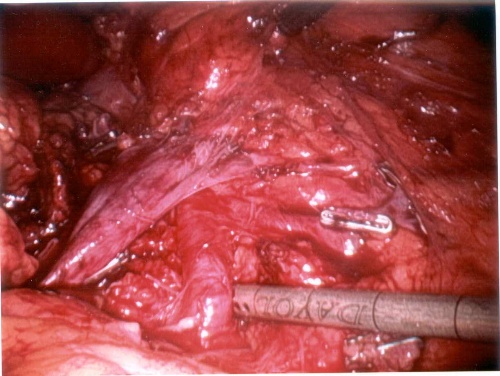
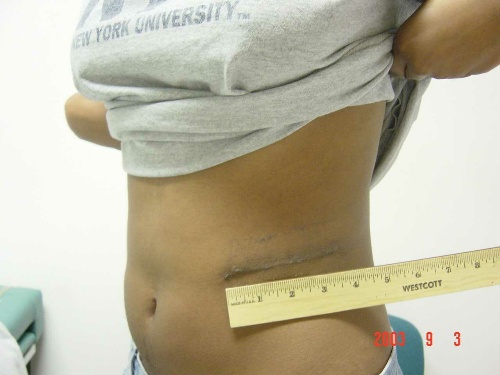 Figure 3. Laparoscopic nephrectomy: intra-operative view of the renal hilum including the renal vein and renal artery (immediately in front of the suction device).
 CONCLUSION Attitudes toward the use of living donors for transplantation have evolved over the past fifty years. Most centers support the use of living donors, because of the favorable risk-benefit ratio and its long-proven success. Widespread support also exists for renal transplantation from an emotionally-related donor (spouse, friend, distant relative, in-law). However, most centers have been unwilling to use strangers as kidney donors. Spital reported that of 126 transplant centers surveyed in 1993, only 15% would accept a kidney from a stranger donor, compared to 62% from a friend and 88% from a spousal donor10. Despite reluctance on the part of transplant centers to entertain the notion of Good Samaritan donation, the practice has gained support from both ethicists and the general public11-13. Indeed, organ donation is an altruistic act and "altruism receives its highest expression in the absence of personal relationships…14". In a recent poll, 80% of respondents supported stranger kidney donation15. Additionally, a surprising number of respondents answered favorably when asked if they would (24%) or probably would (21%) donate a kidney to a stranger in need for free15. Although this remarkable response has not been realized in clinical practice (only a few hundred altruistic donations have actually taken place), it does underscore the resolve of the general public and does imply an underutilized resource for donor kidneys. The failure of the transplant community to fully embrace this notion is puzzling. Given the success of genetically unrelated living donors, it would be indefensible to reject altruistic donors for medical reasons alone, and reduces the debate to a philosophical one. In other contexts, the offer to risk one’s life for the common good (e.g. fire fighters, soldiers, and police officers) would be praised and revered. Yet here, such an extraordinary gesture from a Good Samaritan donor raises deep suspicions of their motives or mental health. Rather than thanking them for their generosity and courage, we invite them to undergo a psychiatric examination. Some of these concerns are certainly understandable. Because living donation by its nature involves exposing an otherwise healthy individual to the risks of surgery, the benefits of the donation must outweigh the risks. In directed donation, there is a defined benefit for the donor who gains the knowledge that they have improved the health or even saved the life of a person with whom they share a relationship, whether genetic or emotional. Inherent in this relationship is a sense of obligation that some family members may feel to improve the welfare of their loved ones. For altruistic donors, the benefits are more heavily weighted by an altruistic standard, since they do not share a relationship or even know the identity of the beneficiary of their actions. This line of reasoning would suggest that seeing a loved one’s life improved or saved is a more rationale justification than the psychological benefit to a stranger performing an altruistic act. The results of the present study should allay some of these biases. While recognizing the limitations of the small sample size, the altruistic donors in this series can be described as well-functioning, well-educated, productive members of society. Short-term follow-up after donation by a health-related quality-of-life survey detected no adverse physical or psychological consequences to the altruistic donors. All had returned to their baseline status (including employment) without any limitations to their activities. This is not at all surprising since there is no compelling reason to suspect that the risk to a stranger donor would differ in any manner from a living-related donor. Furthermore, all individuals expressed great satisfaction in donating a kidney, regardless of whether their recipient had been a stranger. All appeared to be properly motivated by altruism rather than mental illness. A poignant example is our first altruistic donor, an ordained Buddhist monk. When asked her motives for donating a kidney, she simply replied, "because somebody needs it more than I do." Importantly, all donors also spoke of their satisfaction with the information they received from our transplant program, and given similar circumstances, would undergo the procedure again. In line with these encouraging results, our organ procurement organization (the New England Organ Bank) has established a system for addressing potential altruistic donors. A screening interview is arranged for potential donors in which preliminary information and contacts to local transplant centers are provided. The Web site for the organ procurement organization has also been modified to include material about this issue, although no attempts are made to actively solicit potential non-directed donors and relies on the individual to make the initial contact. Furthermore, an educational initiative is currently underway within the region to inform other transplant professionals and local communities about Good Samaritan donation. In this way, we hope to positively influence centers with lingering doubts about the propriety of this practice to at least consider the option of altruistic donation. In so doing, the transplant community may not only honor the goals of those who wish to donate, but also provide an excellent opportunity to alleviate the ever-growing shortage of solid organs for transplantation. REFERENCES
|