
|
Paneles de Discussión
Paneais de Discussio |
The Regional Classification of Parathyroid Tissue as used for Tissue Selection prior to Autotransplantation.Helmut Hörandner and Ulrich NeyerElectron Microscopy Laboratory Mauer, Vienna
|
 |  |
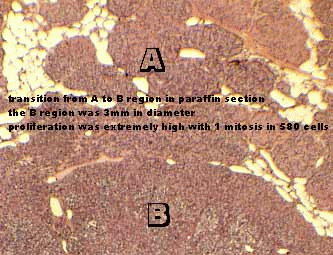
Minimally changed A - regions may show slight hypertrophy (8 - 10000 cells/mm2), and proliferation (one mitosis <40000 cells, MIB - 1 or PCNA activity up to 40 cells/ mm2[yellow in fig 5 and 8]). Intracellular lipid vacuoles are reduced, glycogen still present and mitochondria augmented (fig 4). This may reflect hyperactivity.
B-Regions represent highly hypertrophic/hyperplastic tissue without a visible capsule. Stromal fat cells and intracellular lipid are absent, causing sometimes a whitish colour macroscopically (fig 2). Cells are enlarged (6 - 8000/mm2) and usually arranged in follicles (fig6,10). Mitochondria are abundant , golgi enlarged and branched, endoplasmic reticulum usually arranged in parallel stacks. Highest proliferation rates could be found (up to one mitosis in 300 cells, MIB - 1 or PCNA activity up to 600 cells/ mm2[orange and red in fig 5 and 8]) in confined regions up to 3mm in diameter (fig 3,5). Monomorphic ultrastructure suggests monoclonal origin (fig 6,10). Sinusoidal capillaries can be detected already macroscopically.
Hypertrophy of the cells leads to dramatic reduction in connective tissue content (fig7). B-Regions are almost unsuppressible and cause highest PTH levels in vivo.
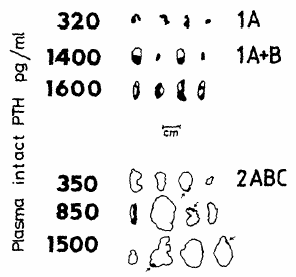
Nodular C-Regions show identical cytologic details as B-Regions and are surrounded by a capsule (fig9). This enables identification with the naked eye. Proliferation is high, usually lower than in B - regions. Cells are usually arranged in follicles, which are sealed by tight junctions (fig10). Their uniform ultrastructure suggests monoclonality, which has been established for large nodules.
PTH-values vivo are lower than in comparable B-glands: the drawings on the left represent the largest cross sections of the parathyroid glands in patients with pure diffuse or nodular gland population (which is rare). The difference may be up to 50times expressed as pg PTH/ mg tissue mass. We found frequently atypical Ca/PTH response curves indicating diminished Ca++ -receptor density (see Cm above).
Nodular D-Regions consist almost exclusively of oxyphil cells, many of them with hypertrophic mitochondria and pycnotic nuclei (fig 13). Macroscopically they are detected by white colour, caused by the hypertrophic mitochondria (fig 11, 12). Ultrastructure is suggestive for apoptosis, although biochemical characterization failed up to now (fig 13). Proliferation is similar or slightly lower than in C-Regions.
Clinical outcome
In the initial period 3 (out of 25 patients) relapses occurred in Vienna, and 3 (out of 8 patients) in Feldkirch.
In the following period only one relapse occurred in Vienna (1987) and in Feldkirch (1992).
No other true relapses occurred. Further reoperations had been necessitated by supernumerary glands, in 2 patients by parathyromatosis in the neck.
A detailed statistically relevant investigation on the long term outcome of total PTx+AT has been presented. (in lit (77) of: parathyroidectomy in renal hyperparathyroidism) .
71.- Hörandner H, Neyer U, Gruber U, et al: Pathomorphologie von autotransplantiertem Nebenschilddrüsengewebe. Nieren- und Hochdruckkrankheiten, 1997; 26: 319-327
72.- Niederle B, Hörandner H, Roka R, et al: Parathyreoidektomie und Autotransplantation beim renalen Hyperparathyreoidismus. I. Morphologische Untersuchungen zur Gewebeauswahl. Langenbecks Arch Chir 1988; 373: 325-336
73.- Niederle B, Hörandner H, Roka R, et al: Parathyreoidektomie und Autotransplantation beim renalen Hyperparathyroidismus. II. Funktionelle Untersuchungen zur Gewebeauswahl. Langenbecks Arch Chir 1988; 373: 337-344
REFERENCES