
|
Paneles de Discussión
Paneais de Discussio |
COULD CHRONIC LEAD POISONING BE A CAUSE OF RENAL INSUFFICIENCY IN PATIENTS WITH HYPERTENSION AND GOUT?Ana I. Sánchez FructuosoNephrology Unit, Hospital Clínico San Carlos, Madrid, Spainsanchezfruct@telefonica.netLead is responsible for one of the most common forms of chronic, silent poisoning in the modern world. For some time, lead poisoning has been recognised as an industrial hazard though it is only recently that its long-term effects as an environmental toxic agent have sparked the interest of researchers because of the variable nature of the disease provoked by the heavy metal. Spain has a high incidence of cases of lead poisoning in the workplace, though it is not clear how many intoxications are produced in the "theoretically non-exposed" general population. Lead nephropathy was described as early as in 1862 1. However, the first observations of significance emerged in Australia over the 1920s. In a detailed comparative study, a substantial increase in the incidence of death due to chronic nephropathy was revealed in Queensland compared to other Australian states. The large number of deaths due to chronic renal insufficiency recorded between 1917 and 1926 in this region was finally attributed to a considerable number of children becoming lead poisoned by licking painted wood railings in their houses 2. This observation was subsequently confirmed by Henderson in the '50s who determined bone lead and mortality through the follow up lead-poisoned children 3. Epidemiological studies in subjects not previously exposed to lead Most studies of lead and renal insufficiency have been conducted on patients exposed to the metal at work 4. In a larger number of reports, lead has been established to cause arterial hypertension, gout and renal insufficiency. When these symptoms appear in someone exposed to lead at work, it is easy to relate these signs to lead poisoning, yet when they occur in subjects with no past history of exposure to lead, it is easy to overlook this possibility in the differential diagnosis. It is nevertheless clear, that lead is a significant environmental pollutant that may affect a large number of people. In effect, there are numerous sources of lead; the water supply perhaps being the most frequent since the metal may be released from pipes, connectors and solders 5. Other common sources include foodstuffs, wine 6 or other alcoholic beverages kept in vessels with high lead contents, earthenware glazed with the metal 7, air pollution including the use of leaded fuel 7, and paint 7, 8. There are data to suggest that lead could be a cause of renal insufficiency, gout and arterial hypertension in the general population. Campbell et al. 9 found high lead levels in water in approximately a quarter of the Scottish homes they examined. The inhabitants of these houses were subsequently found to show a significantly high incidence of high blood urea. Moreover, there have been reports of a higher incidence and prevalence of patients undergoing dialysis in areas of substantial lead-related industry as well as a higher proportion of deaths due to chronic renal disease 10. A higher diastolic blood pressure has also been noted in subjects living in areas of soft water (from which more lead is released) than in residents of hard water regions 11. Inhabitants of soft water areas have also been related to a higher bone lead burden 12. In a large study 13 performed in the USA by the National Health and Nutrition Examination Survey II (NHANES II) from 1976 to 1980 in which plasma lead was determined in close to 10,000 subjects, significant correlation was observed between plasma lead levels and systolic and diastolic arterial pressure. The literature also contains data to support a relationship between lead and renal insufficiency in the general population. In a randomised population of almost 2000 people, Staessen et al. 14 found a significant negative relationship between creatinine clearance and blood lead. Batuman et al. 14 subjected 48 patients with presumed essential hypertension to EDTA mobilisation tests and noted that those with renal insufficiency excreted much higher amounts of lead than those showing normal renal function. Renal insufficiency, gout and arterial hypertension Despite it being evident that malignant hypertension causes kidney damage, whether "benign" hypertension is capable of provoking renal insufficiency is unclear 17,18. Though some clinicians think that benign hypertension is a cause of renal insufficiency, there is really little evidence to support this. Several lines of research have attempted to identify the factors responsible for a proportion of hypertensive patients developing renal insufficiency, among which chronic lead poisoning is a possible factor. Vupputuri et al. 19 recently demonstrated a significant positive link between blood lead and blood pressure in a large Afro-American population. This finding has had important implications for public health. Further, it was observed that these Afro-Americans had high blood lead levels (probably because of their lower socioeconomic status they are more exposed to lead sources) and this could, at least in part, explain the higher incidence of hypertension in this population compared to the Caucasian population. In addition, the fact that end-stage chronic renal insufficiency secondary to hypertension is more common in Afro-Americans is indicative of different mechanisms, including lead intoxication, causing renal damage. The situation is similar for gout nephropathy. Some authors would argue that gout nephropathy does not exist, since follow-up studies performed in the seventies suggested that hyperuricaemia and primary gout rarely progress to renal insufficiency unless there is a further cause of kidney disease, mainly arterial hypertension 20-22. Once again, lead could be the link between gout, hypertension and kidney disease. It should also be remembered that in hypertensive patients, hyperuricaemia is among the factors indicating a worse prognosis for the development of a nephropathy 23. Using the EDTA test, we determined body lead levels in a population of 296 subjects. The subjects were divided into four groups: control healthy subjects (N=30); patients with essential arterial hypertension and normal kidney function referred to hospital because their blood pressure was poorly controlled (N=104); patients with chronic renal insufficiency related to arterial hypertension and/or gout (N=132) and, finally, 30 subjects with renal insufficiency of clearly established cause (glomerulonephritis, polycystosis, etc.). We observed high lead levels in 15% of the hypertensive patients with normal renal function, in 44% of the patients with renal insufficiency presumably secondary to nephroangiosclerosis and in an incredible 69% of our patients with renal insufficiency presumed secondary to gout 24. 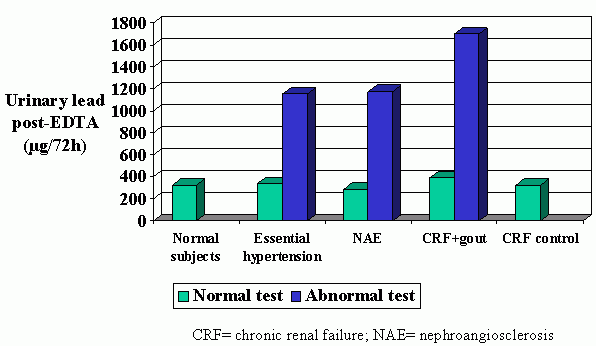
In summary, it seems that chronic exposure to low environmental lead levels could pose a serious public health problem in that it may cause hypertension, gout and renal insufficiency. Thus, subjects presenting with these clinical symptoms should be first checked for lead poisoning. REFERENCES
|