
|
Paneles de Discussión
Paneais de Discussio |
When to start dialysisJames TattersallLeeds, UKIntroduction The outcome for dialysis patients in terms of survival, morbidity and quality of life is very poor (Figure 1), especially in elderly patients with co-morbidity (e.g. diabetes). The mortality of dialysis patients is particularly high in the first months after dialysis has started. The desire to reduce this mortality motivates the discussion on when to start dialysis. There is now overwhelming evidence in dialysis patients that a small solute clearance lower than around 8% of normal renal function (Weekly Kt/V < 1.6 by Haemodialysis or per-session Kt/V < 0.9) is associated with increased mortality. Higher doses than this are considered optimal. There is also overwhelming evidence in dialysis patients that malnutrition (represented by a variety of markers including nPNA < 0.8 g/Kg/24h and albumin <35g/dL) is associated with an increased mortality. In the period before dialysis starts, small-solute clearance and nutritional markers gradually decline. Typically, these markers increase after dialysis starts. It is theoretically possible that some of the mortality in dialysis (particularly the early mortality) may be related to preventable factors including uraemia and malnutrition before dialysis starts. By starting dialysis earlier, some of this initial uraemia and malnutrition may be avoided and there is the prospect that mortality may be reduced. On the other hand, the dialysis process itself is bio-incompatible un-physiological and may be associated with side effects which could offset any advantage in starting dialysis early. Key evidence relating overall outcome or mortality to the timing of dialysis initiation is lacking. Therefore this debate must be informed by theory and indirect evidence. Nevertheless, we cannot avoid making the decision on when to start dialysis in any of our patients with end-stage renal failure. An understanding of the issues is required to inform this vital and life-changing decision. 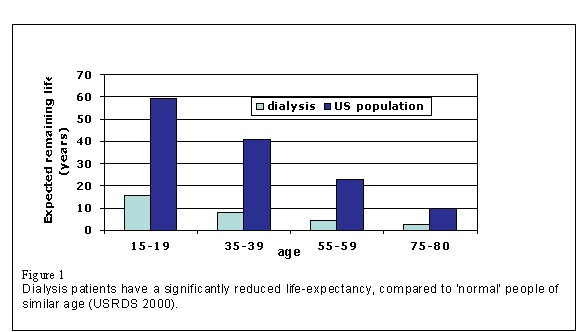
The function of dialysis is to replace the failing renal function so that the patient remains healthy. Dialysis is started when the renal function is inadequate to maintain health. If the decision is based on an assessment of failing health, then dialysis will inevitably be started when the patient’s health has already been damaged by uraemia. This approach is no longer recommended. It makes no sense to allow the patient to suffer detrimental effects of uraemia or malnutrition before ‘rescuing’ them by dialysis. The decision on when to start dialysis must, therefore, be informed by measurements or estimation of the renal function. Ideally, dialysis is started before the renal function has declined to a level, which places the patient at risk of uraemic symptoms or damage. While many of the functions of the failing kidney (e.g. haemoglobin and blood pressure homeostasis) can be supported or replaced without dialysis, the excretory and base regeneration functions cannot. Therefore, the timing of the start of dialysis must mainly be guided by measurement of clearance, acid-base and volume status. Clinical symptoms are unreliable as they are subjective and prone to bias. They also tend to occur late in the progression of renal failure and be non-specific. Blood urea and creatinine Renal function cannot be quantified by simple measurements of urea and creatinine in the blood. This is because the blood level is determined equally by renal function and by its generation rate. Without knowledge of the generation rate, the blood levels cannot be interpreted. Urea is generated by the liver from excess dietary nitrogen. As renal function declines, the patient spontaneously restricts his dietary nitrogen intake and urea generation falls. Therefore, the serum urea concentration tends not to rise as renal failure progresses. Urea concentrations may even fall due to anorexia in advanced uraemia. Creatinine is generated from muscles and its generation rate is determined by muscle mass, activity and, to a lesser extent, dietary protein intake. As renal function declines, the creatinine generation rate tends to fall due to inactivity. Therefore, the serum creatinine level tends not to rise beyond a certain point as renal failure progresses. The creatinine generation tends to be higher in males than in females (due to a relatively higher muscle mass) and in certain racial groups (e.g. American Blacks). If serum creatinine (or reciprocal creatinine) is used to guide the decision on when to start dialysis, males will be selected at an earlier stage of their renal failure than females. This may partly explain the reason for a higher proportion of males than females in dialysis patients in certain regions. For these reasons, current guidelines recommend measurements or estimations of glomerular filtration rate (GFR) normalised to surface area. Serum creatinine or reciprocal creatinine should not be used to guide the decision on when to start dialysis. Additionally, some guidelines recommend quantifying renal function as weekly urea clearance, normalised to body water volume (Kt/V). This makes some sense to nephrologists who measure Kt/V in peritoneal dialysis patients, but may confuse non-nephrologists or those who measure Kt/V in haemodialysis. In haemodialysis, Kt/V is a different measure of clearance and cannot easily be compared to the Kt/V of peritoneal dialysis or renal function. More recent guidelines tend to emphasise GFR as the main measure of renal function. Although serum creatinine on its own cannot be used to quantify renal function, it can be used to screen for renal failure, provided sex is taken into account. The cut-off value for a clearance of less than 60 ml/min/1.73 m2 (which represents significant renal damage) is 137 micromol/liter for men and 104 micromol/liter for women. For a clearance of less than 30 ml/min/1.73 m2 (which represents severe renal damage) the cut-off value is 177 micromol/liter for men and 146 micromol/liter for women.
Creatinine clearance may be calculated from 24h urine collections and serum creatinine. It has commonly been used in the past to quantify renal function. Creatinine clearance is higher than GFR due to tubular excretion of creatinine. The difference depends on GFR. At normal renal function, creatinine clearance is around 20% higher than GFR. At around 10% of normal renal function (the level at which dialysis may be considered), creatinine clearance is around twice GFR as tubular creatinine excretion is relatively preserved. Because creatinine overestimates GFR, particularly when renal failure is severe, it should no longer be used to quantify renal function. The Cockcroft and Gault method predicts creatinine clearance from weight, age, sex and serum creatinine and also should not be used. How to measure GFR GFR may be calculated from the rate of fall in blood concentration of an injected tracer. This is the most accurate method but generally considered to be too invasive and complicated for routine use. GFR can be calculated from measurement of urea, creatinine and volume in a 24h urine collection and the serum urea and creatinine. Urea is absorbed from the renal tubules and urea clearance tends to underestimate GFR by about the same amount as creatinine clearance overestimates GFR. The mean of urea and creatinine clearance has been shown to be close to GFR. The urine collection method is accurate if the collection is performed properly (start collection from an empty bladder, collect all urine passed up to and including a complete voiding exactly 24 hours after start). Patients may incorrectly start the collection with a full bladder, which results in a significant overestimation. Urine collection methods for calculating GFR require correction for surface area. Results reported from the lab are generally uncorrected. Calculation of GFR from urine collections; GFR=Glomerular filtration rate in mL/min/1.73m2, SA=surface area in m2, t=duration of collection in minutes (usually 1440), Uvol= urine collection volume in mL, Uurea, Ucreat= urine urea and creatinine concentrations. Surea, Screat=serum urea and creatinine concentrations. Urea and creatinine concentrations must be in same units for urine and serum.
Calculation of surface area, preferred method (Gehan & George) SA in m2, weight in kg, height in cm.
How to predict GFR using serum creatinine There are a number of different methods for predicting (calculating) GFR from serum creatinine. All methods make allowance for the different rates of creatinine generation in individual patients. Creatinine generation rate is influenced by dietary protein intake, muscle mass and activity. The GFR prediction methods attempt to allow for this variation by using the patients sex and age. The accuracy of the prediction is increased by serum albumin in certain versions of the MDRD equations and by weight in the Cockroft and Gault equation. If the patient has lower than average (for age and sex) muscle mass or protein intake, then the predicted GFR will be over-estimated. The Cockcroft and Gault method has been used commonly in the past. This predicts uncorrected creatinine clearance (not GFR). It significantly overestimates GFR, particularly at low GFR and should no longer be used. The MDRD method has been validated in patients with low clearance and was developed to return GFR1 . It has been shown to be at least as accurate as the urine collection method. The MDRD method returns a GFR, which is already corrected for surface area. Since the MDRD method requires only data, which is available to the laboratory (no weight is required), it is recommended that the laboratory report GFR directly.
Calculation of GFR from age, gender, race, urea, creatinine and albumin (MDRD equation). Albumin in g/dL, age in years. GFR in mL/min/1.73m2. Validated in US white and black (Afro-Caribbean) patients. Multiply by 1.18 if patient is black. Multiply by 0.762 if patient is female. SI units (Creat in µmol/L, Urea in mmol/L)
US units (Creat in mg/dL, BUN in mg/dL)
Problems with predicting GFR from serum creatinine All methods for predicting GFR from serum creatinine depend on an assumption of creatinine generation based on age, sex and other variables. There will always be patients whose creatinine generation rate varies significantly from the predicted. In this case the predicted GFR will be incorrect. Of particular concern are the elderly, inactive patients with low muscle mass – termed sarcopenia. These patients may also have malnutrition and arterial disease and have a high mortality rate2. Patients with sarcopenia have a low creatinine generation rate and the GFR will be greatly overestimated by the prediction equations, especially at low GFR3 . Methods for calculating GFR from urine collections or tracer are not affected by sarcopenia.
Small solute clearance by dialysis is typically around 10% of normal renal function. (Figure 2). Small solute clearance below this minimal level has been associated with reduced survival in numerous studies in both HD and PD. In theory, there should be benefits from increasing clearance above this minimum level. However this expectation has not been confirmed by evidence. There are practical difficulties in increasing this ratio by thrice weekly haemodialysis or CAPD. In thrice-weekly haemodialysis, once Kt/V has reached 1.2 (equivalent to around 12% of normal renal urea clearance), further increases, have minimal impact on the pre-dialysis urea level. Once the post-dialysis urea has been reduced to low levels by intermittent haemodialysis, the pre-dialysis levels are determined mainly by generation in the interval between dialysis sessions. Unless haemodialysis frequency is increased, there is little scope for increasing clearance. In peritoneal dialysis, urea clearance is limited to around 20ml/min by the peritoneal mass transfer area coefficient. There are practical difficulties in approaching 20ml/min as it would require fluid exchanges of much more than 30 litres per day. If low clearance levels are considered to be harmful in dialysis patients, it makes sense to avoid these low levels in the period before dialysis starts also. Using this logic, we should start dialysis at a GFR around 10 ml/min, equivalent to a weekly urea Kt/V of 2 and creatinine clearance 12 ml/min. As practical problems, which limit the efficacy and safety of dialysis, are overcome in the future, higher doses of dialysis may prove to be desirable. In this case dialysis should be started at an earlier stage, to match the optimal level for dialysis. Nutrition Dietary protein intake spontaneously falls as renal failure progresses. There is evidence that nutrition is already compromised when GFR drops below 50ml/min (Table1). 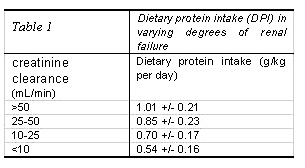 When dialysis is started at GFR around 6 ml/min, the dietary protein intake is more seriously reduced and tends to increase after dialysis starts. There is evidence in CAPD patients that patients who start dialysis with very low GFR never recover their nutritional state to match those who started with higher GFR. Markers of nutrition when dialysis is started, such as serum albumin and protein nitrogen appearance, are a powerful predictor of mortality on dialysis. On the nutritional evidence, one should not wait for signs of malnutrition before starting dialysis, since this would subject the patient to an increased risk of death. Acid/base status One of the functions of the human kidney is to regenerate bicarbonate. Dialysis achieves this by including a supra-physiological concentration of bicarbonate or (metabolic equivalent) in the dialysis fluid. Optimal survival has been shown to relate to normal pre-dialysis serum bicarbonate concentration. Metabolic acidosis has the potential for causing malnutrition. Increasing the blood bicarbonate in haemodialysis and CAPD patients has been shown to increase nutritional markers. Metabolic acidosis also causes osteomalacia. There have been few studies in the pre-dialysis period but in dialysis patients, a time-averaged serum bicarbonate of 24mM is considered to be the gold standard of optimal control 4. In theory, normal serum bicarbonate may be achieved without dialysis in severe renal failure by treatment with oral sodium bicarbonate. However, this involves a significant sodium load, which may conflict with treatment of fluid overload and blood pressure. In practice, metabolic acidosis should be taken as an indication that dialysis should be started. In my experience, patients with metabolic acidosis generally qualify for starting dialysis on other criteria and treatment with oral bicarbonate in these patients is hardly ever needed except when there is also a renal tubular bicarbonate wasting state. Salt/water balance, hypertension and cardio-vascular risk. Left ventricular hypertrophy (LVH) is known to be a powerful predictor of death in dialysis patients5. If it is present at the start of dialysis, it is a powerful predictor of poor survival on dialysis6. The majority of deaths on dialysis, at least during the first few years, is caused by cardiac disease and LVH is thought to be a major factor in these deaths. LVH tends to develop relatively early in the course of the renal failure7 and is normally established when dialysis starts (Table 2)5. 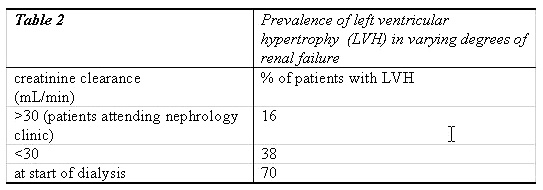 Attention to the causes of LVH in the pre-dialysis period has a dramatic impact on the survival of dialysis patients8. Treatment with ACE inhibitors has been shown to prevent development and cause regression of LVH 9, 10, 11. Prevention of LVH in the pre-dialysis period includes aggressive blood pressure control, use of ACE-inhibitors or angiotensin receptor blockers, prevention of anaemia and attention to fluid overload. In renal failure, hypertension is usually due to a combination of activation of the renin-angiotensin system and chronic fluid overload. Inability to control hypertension or fluid overload, despite high doses of diuretic or appropriate drugs, is an indication to start dialysis. ACE inhibitors or angiotensin receptor blockers should be used where possible even when the renal function is critically low. Evidence There have been no randomised, prospective controlled trials designed to provide evidence on when to start dialysis. Dialysis is currently started when GFR is at a mean of around 6 mL/min but there are wide variations with some groups advocating starting with a GFR of 15 mL/min. Numerous retrospective observational studies have suggested a reduced survival in patients starting dialysis later than at a GFR of 6 ml/min compared to starting dialysis earlier12. These studies may be criticised for failing to control for the effects of late referral, which may be an independent risk for dialysis mortality. The Netherlands Cooperative Study on the Adequacy of Dialysis suggested that a patient survives around 2.5 months longer if started on dialysis according to the DOQI guidelines (GFR >10 mL/min or nPNA>0.8 g/Kg/day) compared to a later start. This survival advantage was considered by the study authors to be due to the patients starting dialysis at an earlier stage in their disease, estimated at around 4 months13. The latter study was retrospective, the patients were relatively young and disease progression in the period before dialysis started was not studied. Analysis of registry data suggest that patients starting dialysis ‘early’ with higher predicted GFR have significantly higher mortality than those started ‘late’ with lower GFR. The same data shows that the relationship is even stronger between inverse serum creatinine and mortality. There is a strong association between low serum creatinine at the start of dialysis and subsequent mortality. This relationship is likely to be caused by low creatinine being a marker for sarcopenia. GFR is known to be overestimated by prediction equations in this situation. Sarcopenia is associated with malnutrition, low muscle mass, inactivity and cardiovascular disease. It carries a very high mortality rate. Studies measuring renal function using urine collections (which are not subject to this overestimation in sarcopenia) do not show this relationship between mortality and renal function 14. 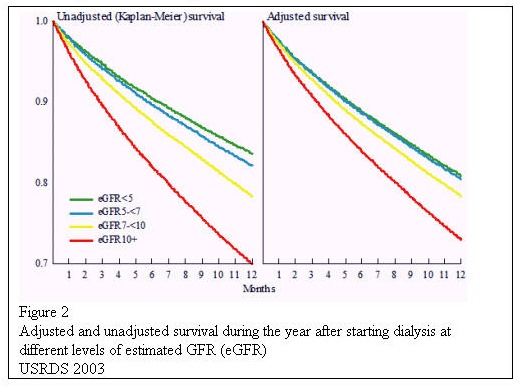 There are also suggested and theoretical benefits of starting dialysis earlier than a GFR of 10 mL/minute15. In the CANUSA study of CAPD patients a combination of renal and dialysis creatinine clearance of greater than 10 mL/min was associated with a significantly improved survival16. Since most of the variability in total clearance in the CANUSA study was due to the initial residual renal function, this suggests that the higher the residual renal function at the start of dialysis, the better the outcome. While the optimal level of GFR for starting dialysis remains controversial, there is no data supporting the safety of delaying dialysis until the patient is symptomatic with a GFR below 6 mL/min. Conclusion and guidelines A fit patient with chronic renal failure attending a clinic is likely to be far cheaper to manage than a patient who has been established on dialysis. His quality of life is also likely to be better. If dialysis is started unnecessarily early then costs would increase and quality of life decrease. However, the cost-savings and quality of life benefit resulting from a delayed start to dialysis may be cancelled out by increased morbidity or hospitalisations17. The published data often fails to separate the effect of delayed referral and delayed dialysis. There is now evidence that delayed referral carries a higher mortality and cost than appropriate early referral. Patients referred late also tend to start dialysis late but it is not clear whether this is higher mortality is due to inadequate care in the pre-dialysis period or to late initiation of dialysis. In my opinion, it is more important to provide appropriate early care in the pre-dialysis period than to start dialysis early. This appropriate pre-dialysis care includes the correction of anaemia, hypertension, calcium-phosphate abnormalities, fluid overload and acid base abnormalities. At present, there is no clear consensus on when dialysis should start. The confusion may be exploited by the patient who will often be in denial of the existence of his or her renal failure or unaware of its consequences and will pressurize the physician to delay the start of dialysis. In capitated or systems other than fee-for-service, hospital managers may also pressurize the physician to delay the start of dialysis for economic reasons, unaware or unconvinced of the hidden cost of delayed start. For these reasons, it has become imperative that objective data is applied to guide the selection of the most appropriate time to start dialysis. We need to judge the start of dialysis at that point just before the patient develops any observable adverse effect of uremia including malnutrition. The level of renal function at which dialysis should be started is a dynamic quantity. Dialysis should be started at the point at which the adverse effects of delaying dialysis further outweighs the adverse effects and disadvantages of the dialysis itself. As our ability to deliver safer, better tolerated and more powerful dialysis increases, the level of renal function at which dialysis is started will also increase. In general, this level will be close to the level considered as the minimum acceptable equivalent clearance for dialysis patients. The year 2000 US DOQI guidelines recommend starting dialysis when Kt/V falls below 2.0 (GFR 14 ml/min/1.73m2) and nPNA less than 0.8 g/Kg/24h. The year 2002 European Best Practice Guidelines recommend starting dialysis when GFR falls below 14 ml/min/1.73m2, especially if there is malnutrition, fluid overload, acidosis or hypertension despite treatment. In any case dialysis should be started before GFR drops below 6 ml/min/1.73m2, even if there are no symptoms or signs. Although guided by objective measurement and current guidelines, the actual decision to start dialysis is the result of a subjective assessment of the impact of uremia and dialysis on the patient’s life. The informed patient is best placed to make this decision.
References
| |||||||||||||||||||||||||||||||||||||||||||||||||||||||