
|
Paneles de Discussión
Paneais de Discussio |
IS RECOMBINANT-HUMAN ERYTHROPOIETIN RESISTANCE ANOTHER PREDICTOR OF CARDIOVASCULAR DISEASE IN END-STAGE RENAL FAILURE PATIENTS? PARASKEVI TSEKE, MD AND GEORGE TSIRPANLIS, MD
RENAL UNIT, ALEXANDRA GENERAL HOSPITAL, ATHENS, GREECE Introduction Cardiovascular disease (CVD) is the major cause of morbidity and mortality in patients with end-stage renal failure (ESRF) 1. Traditional (age, gender, hypertension, diabetes, dyslipidemia) and nontraditional (homocysteine, inflammation, oxidant stress etc) or emerging risk factors are considered to be the causes of atherosclerotic CVD in this high-risk population 2.
Anemia in ESRF patients is considered to be an independent risk factor for heart failure upon dialysis initiation, whereas it can also predict the recurrence of heart failure at a later stage 3. Erythropoietin (EPO) deficiency has been recognized as the main cause of anemia in ESRF and the introduction of recombinant human erythropoietin (rHuEpo) in the late 1980s significantly improved its management. Almost 90% of patients receiving rHuEpo respond to treatment and they achieve target hemoglobin (Hb) levels. Nevertheless, a large number of patients show "hyporesponsiveness" or "resistance" to rHuEpo. Resistance to recombinant human Erythropoietin treatment According to the European Best Practice Guidelines and the US Guidelines resistance to rHuEpo is defined as inappropriate response to treatment with doses >300 IU/kg/week, when administered subcutaneously, or >400 IU/kg/week and 450 IU/kg/week, respectively, when administered intravenously 4, 5. Among causes of hyporesponsiveness to rHuEpo the most common one is iron deficiency, either functional or absolute. Other conditions involved in rHuEpo resistance are shown in table 1. Table 1
Could rHuEpo resistance be related to atherosclerotic CVD in ESRF patients? We consider that some factors of the former entity are common or related to the later one. We will try to explore these common factors and the probable pathogenetic mechanisms correlating atherosclerotic CVD to rHuEpo resistance in ESRF patients. RHuEpo resistance conditions related to CVD risk
As mentioned above anemia is directly related to the development of heart failure in ESRF patients. Anemia is associated with hypoxia, which may lead to left ventricular hypertrophy, myocardial fibrosis, cardiomyopathy and congestive heart failure 6 Furthermore, erythrocytes are considered as mobile free radical scavenges, providing not only oxygen, but antioxidant defense systems (eg enzymes of glutathione synthesis and the oxidative pentose phosphate pathway, superoxide dismutase, tocophenols, ascorbic acid) and they are able to reach at any tissue or organ exposed to oxidative stress. In renal failure there is marked reduction in antioxidant and mobile free radical scavenger capacity, due to reduced red cells number and lifespan and increased oxidative stress associated with uremia per se, dialysis procedure and alterations in ATP turnover and neuroaminidase activity 7 Thus, anemia per se, the rHuEpo major consequence could contribute to cardiovascular disease and to oxidant stress induction – an emerging CVD risk factor - via antioxidant defense reduction. Iron deficiency is the most common cause of rHuEpo resistance 4 and iron supplementation is recommended in order to achieve upper limits of ferritin levels in HD patients. In this population, intestinal iron absorption is reduced even in iron-deficient patients and intravenous iron (IV) preparations are usually administered. IV iron supplementation induces oxidative stress, LDL and other molecules oxidation, endothelial dysfunction and probably hemochromatosis by iron overload. 8 Some studies have detected a positive correlation between intravenous iron supplementation and oxidative stress induction. Intravenous iron administration in HD patients has been shown to correlate with increased protein oxidation and inflammation as assessed by elevated CRP and TNF-α levels 9. Additionally, a correlation between serum ferritin level and low-density lipoprotein oxidation has been detected, suggesting that iron could promote lipid peroxidation 8. Furthermore, iron seems to correlate with endothelial dysfunction possibly through impairment of nitric oxide activity 8. Oxidative stress induction and its consequences, nitric oxide activity disturbances and endothelial dysfunction are factors, which contributes to the initiation and progression of atherosclerosis.
Homocysteine is a sulfur amino acid whose metabolism depends on Vit B12 and folic acid. Vitamin B12 and folate levels are often low in patients undergoing HD while homocysteine is much more increased than in general population 10. Homocysteine, is a potential independent risk factor for atherosclerosis in the general population. Serum creatinine is a strong determinant of homocysteine levels 11. High dose folate (5-15 mg) reduces the serum concentration of homocysteine. Some experimental and clinical studies have detected an improvement in endothelial function, by reducing homocysteine with folate supplementation 11. Thus vitamin B12 and folate deficiency via hyperhomocysteinemia are concomitantly risk factors for rHEpo resistance and CVD appearance. Inflammatory indices are increased in ESRF patients; the inflammatory state in these patients is due to factors related to uremia itself, to dialysis procedure and possibly to co-morbidities that they present (atherosclerosis, diabetes, sub-clinical infections, advanced age etc). Oxidative stress is another factor possibly interrelated to inflammation in HD patients (12, 13. Inflammatory cytokines can directly inhibit red cell production by suppressing erythroid colony-forming units and indirectly by impairing iron availability. The second one can be mediated through down regulation of transferring receptors in erythroid cells along with increased expression of lactoferrin receptors, which in turn causes increased iron uptake by tissue macrophages 14 RhuEpo resistance induced by oxidative stress is possibly mediated through direct suppression of erythroid progenitor cells, oxidative damage of red blood cells (RBC) membrane – reducing RBCs survival- increased lipid peroxidation in erythrocytes and impaired iron availability 14, 15, 16, 17 It is questionable how EPO interferes with oxidative stress. Some studies have shown that EPO has antioxidant properties 18, 19, 20, 21 and others that increases the need for antioxidant treatment due to increased consumption of vitamin E, and this is one of the adverse effect correlated with high doses, frequently used in rHuEpo resistance 15. Atherosclerosis is an inflammatory process. Recently, many clinical studies showed that low-grade inflammation could predict atherosclerotic CVD. The already existed or by IV iron supplementation or other causes induced inflammation – and oxidant stress - might be a risk index not only for rHuEpo resistance, but also for atherosclerotic CVD. Furthermore, as recent experimental studies showed inflammation might be a risk factor 22, 23 rather than only a risk index for atherosclerosis initiation and progression. Secondary hyperparathyroidism is a common complication of ESRF. An inverse relation between intact Parathormone (PTH) levels and rHuEpo resistance has been detected in patients undergoing HD. PTH can directly inhibit erythropoesis via inhibition of EPO synthesis, bone marrow erythroid progenitor’s suppression and indirectly via marrow fibrosis24 Furthermore, there is evidence that secondary hyperparathyroidism in ESRF patients correlates with CVD, especially myocardial infarction and congestive heart failure, mediated through increased intracellular calcium in myocytes, vascular and valvular calcification, impaired vascular reactivity, and direct toxic effects of PTH on myocardium (cardiomyopathy, left ventricular hypertrophy and fibrosis) 3, 25 Although recent conclusions from the HEMO study showed that moderately increasing dialysis adequacy cannot influence morbidity and mortality in HD patients, inadequate dialysis is identified as an important factor of poor response to rHuEpo 26 in HD patients. Dialysis dose and frequency are related to the removal of uremic inhibitors of erythropoesis, whereas bioincompatibility of dialysis membranes plays an important role in anemia and rHuEpo resistance, independently of dialysis adequacy. 26 Secondly, extracorporeal circuit correlates with mechanical injury of red cells and haemolysis. On the other hand, dialysis adequacy is possibly correlated to morbidity and mortality – the cardiovascular one is the more significant – that HD patients present 27. Additionally, bioincompatible dialysis membranes have been associated with cardiovascular risk due to increased monocyte activation and production or release of pro-inflammatory and inflammatory cytokines 27. Thus it seems also that inadequate dialysis and possibly bioincompatibility is another common risk factor for rHEpo and cardiovascular morbidity and mortality in HD patients. Malnutrition is a common problem in ESRF patients. It is a potential rHEpo factor. The recently described MIA (Malnutrition-Inflammation-Atherosclerosis) syndrome correlates increased inflammatory to decreased nutritional indexes and atherosclerosis in ESRF patients. Thus malnutrition and inflammation could be common and interrelated risk factors both for CVD and rHEpo 28. Conclusions Although the hypothesis of the present lecture is paradoxical, literature data seem to confirm this suggestion. Many causative factors of rHEpo are also CVD risk factors. These later are the non-traditional or emerging atherosclerotic CVD factors that probably are more significant for this disease prevalence in populations like ESRF patients than in general population. Fig 1 summarizes correlations between rHEpo – CVD and causative or risk factors. An ESRF patient resistant to rHEpo treatment seems to have also a greater risk for CVD than a responder to this treatment. The cause is the existence of common factors that could provoke both entities. 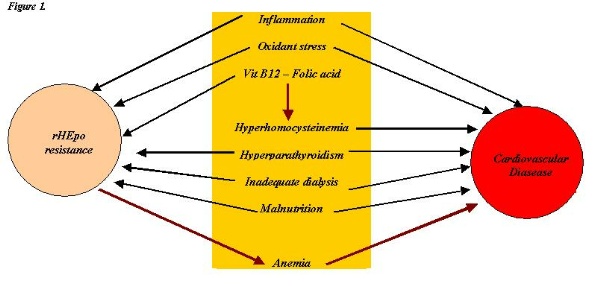
1) Foley RN, Parfey PS, Sarnak MJ. Epidemiology of cardiovascular disease in chronic renal disease. J Am Soc Nephrol 1998; 9: S16-S23 2) Prichard S. Risk factors for coronary artery disease in patients with renal failure. Am J Med Sci 2003; 325: 209-213 3) Locatelli F, Bommer J, London GM, Martin-Malo A, Wanner C, Yagoob M, Zocalli C.Cardiovascular disease determinants in chronic renal failure: clinical approach and treatment. Nephrol Dial Transplant. 2001 Mar; 16(3): 459-68. 4) European Best Practice Guidelines for the Management of Anaemia in Patients with Chronic Renal Failure. Nephrol Dial Transplant. 1999; 14[Suppl 5]: 1-50 5) NFK-DOQI Clinical Practice for the Treatment of Anaemia of Chronic Renal Failure. Am J Kidney Dis 1997; 30[Suppl 3]: S192-S240 6) Silverberg D.Outcomes of anaemia management in renal insufficiency and cardiac disease Nephrol Dial Transplant 2003; 18[Suppl 2]:ii7-ii12 7) Siems WG, Sommerburg O,Grune T: Erythrocyte free radical and energy metabolism. Clin Nephrol 2000; 53[Suppl 1]:s9-s17 8) Kletzmayr J, Hőrl WH:Iron overload and cardiovascular complications in dialysis patients.Nephrol Dial Transplant 2002;17[Suppl 2]:25-29 9) Tovbin D, Mazor D, Vorobiov M, Chaimovitz C, Meyerstein N: Induction of protein oxidation by intravenous iron in hemodialysis patients: Role of inflammation. Am J Kidney Dis 2002;40 (5):1005-1012 10) Bostom AG, Lathrop L. Hyperhomocysteinemia in end-stage renal disease: prevalence, etiology, and potential relationship to atherosclerosis outcomes. Kidney Int 1997; 52: 10-20 11) Brattstrőm L, Wilcken D: Homocysteine and cardiovascular disease: cause or effect? Am J Clin Nutr 2000;72:315-323 12) Nguyen-Koa T, Massy ZA, Pascal de Bandt et al Oxidative stress and hemodialysis: role of inflammation and duration of dialysis treatment. Nephol Dial Transplant 2001; 16: 335-340 13) Stenvinkel P, Barany P: Anaemia, r HuEPO resistance, and cardiovascular disease in end-stage renal failure: links to inflammation and oxidative stress. Nephrol Dial Transplant. 2002; 17[Suppl 5]:32-37. 14) Eckardt KU: Anaemia of critical illness-- implications for understanding and treating rHuEPO resistance Nephrol Dial Transplant. 2002;17 Suppl 5:48-55 15) Usberti M, Gerardi G, Micheli A, Tira P et al Effects of vitamin E-bonded membrane and glutathione on anemia and erythropoietin requirements in hemodialysis patients. J Nephrol 2002;15:558-564 16) Kato A, Odamaki M, Takita T, Furuhashi M, Maruyama Y, Hishida A. High blood soluble receptor p80 for tumour necrosis factor-alpha is associated with erythropoietin resistance in haemodialysis patients. Nephrol Dial Transplant. 2001 Sep;16(9):1838-44. 17) Hirayama A, Nagase S, Gotoh M, Ueda A, Ishizu T, Yoh K, Aoyagi K, Terao J, Koyama A: Reduced serum hydroxyl radical scavenging activity in erythropoietin therapy resistant renal anemia. Free RadicRes 2002; 36(11):1155-1161. 18) Sommerburg O, Grune T, Hampl H, Riedel E, Kuijk F, Ehrich H, Siems WG : Does long-term treatment of renal anaemia with recombinant erythropoietin influence oxidative stress in haemodialysed patients? Nephrol Dial Transplant. 1998; 13:2583-2587. 19) Sommerburg O, Grune T, Hampl H, Riedel E, Ehrich H, Siems WG: Does treatment of renal anemia with recombinant erythropoietin influence oxidative stress in haemodialysis patients? Clin Nephrol 2000; 53[Suppl 1]:s23-s29 20) Calo LA, Stanic L, Davis PA, Pagnin E, Munaretto G, Fusaro M, Landini S, Semplicini A, Piccoli A: Effect of epoetin on HO-1 mRNA level and plasma antioxidants in hemodialysis patients. Int J Clin Pharmacol Ther 2003;41(5):187-192 21) Chen HC, Tsai JC, Tsai JH, Chai YH. Recombinant human erythropoietin enhances superoxide production by FLMP-stimulated polymorphonuclear leukocytes in hemodialysed patients. Kidney Int 1997;52:1390-1394 22) Verma S, Wang C-H, Li S-H, Dumont AS, Fedak PWM, Badiwala MV, Dhillon B, Weisel RD, Li R-K, Mickle DAG, Stewart DJ: A self-fulfilling prophecy. C-reactive protein attenuates nitric oxide production and inhibits angiogenesis. Circulation 2002; 106: 913-919 23) Wang C-H, Li S-H, Weisel RD, Fedak PWM, Dumont AS, Szmitko P, Li R-K, Mickle DAG, Verma S: C-reactive protein upregulates angiotensin type 1 receptors in vascular smooth muscle. Circulation 2003; 107: 1783-1790 24) Drueke T.Hyporesponsiveness to recombinant human erythropoietin :Nephrol Dial Transplant 2001; 16 [Suppl 7]: 25-28 25) Boer I, Gorodetskaya,Young B, Hsu C, Chertow G: The severity of secondary hyperparathyroidism in chronic renal insufficiency is GFR-dependent, race-dependent, and associated with cardiovascular disease. J Am Soc Nephrol 2002; 13:2762-2769 26) Locatelli F, Vecchio L, Andrulli S: Dialysis: its role in optimizing recombinant erythropoietin. Nephrol Dial Tranplant 2001; 16 [Suppl 7]:29-35) 27) Movilli E, Adequacy, nutrition, and biocombatibility: their relevance on clinical outcome in haemodialysis patients, Blood Purif 1999; 17(2-3): 159-65. 28) Stenvinkel P, Heimburger O, Paultre F et al Strong association between malnutrition, inflammation, and atherosclerosis in chronic renal failure. Kidney Int; 55: 1899-1911). |